
Pathology Guide
Explore Oakridge Massage’s comprehensive Pathology Guide to better understand various conditions and how massage can support your health and well-being. Tailored for both clients and practitioners, this resource provides valuable insights into effective treatment options.
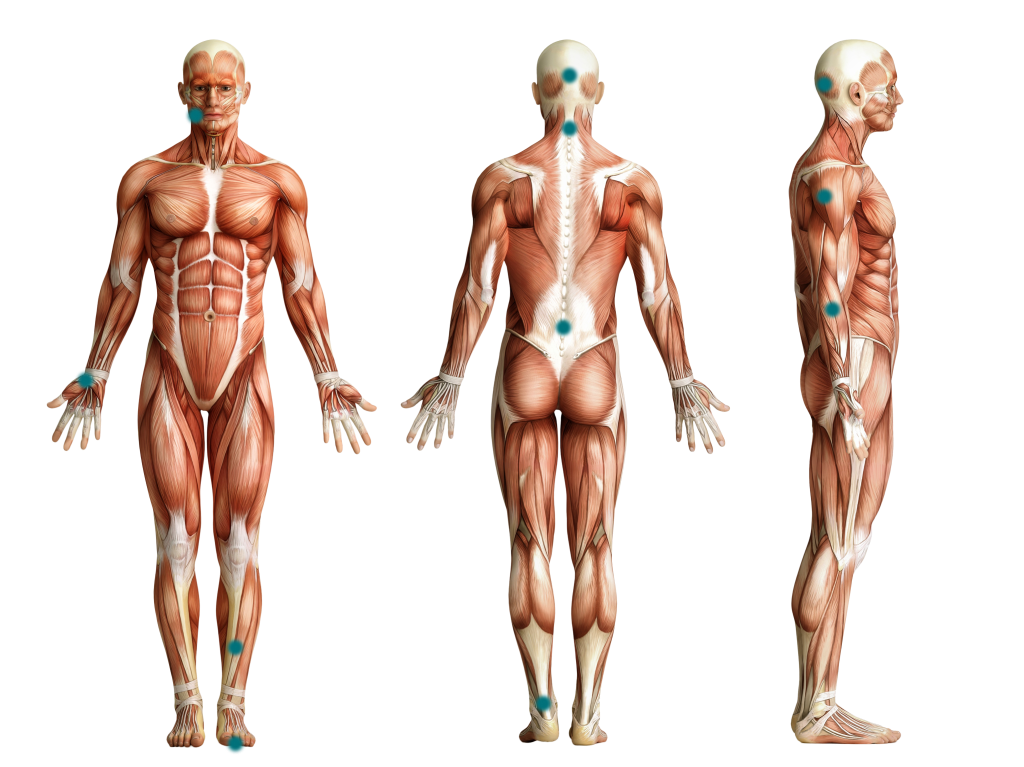
Cervical Region
Upper Extremities
Lumbar Region
Lower Extremities
Causes
网球肘是由前臂肌肉反复承受压力和过度使用引起的,导致连接至外上髁(肘部外侧)的肌腱出现微小撕裂。常见原因包括:
- 重复的手臂动作:网球、刷油漆、打字和使用工具等活动会对前臂肌肉和肌腱施加压力。
- 不正确的技术:在涉及抓握和扭转动作的运动(如网球)或活动中,使用不正确的技术或设备会增加肘部肌腱的负担。
- 年龄:网球肘最常见于30到50岁之间的人群,因为随着年龄增长,肌腱的弹性下降,更易受伤。
Symptoms
网球肘的主要症状是肘部外侧疼痛,但也可能包括:
- 疼痛或灼烧感:疼痛从肘部外侧向前臂延伸,尤其在抓握、提举或扭转时明显。
- 无力:前臂力量下降,握物或提举变得困难。
- 压痛:肘部外侧触感敏感。
- 僵硬:早晨或休息后肘部活动困难,无法完全伸直。
Special Tests RMTs Can Use
RMT可以使用以下测试来评估网球肘:
- Cozen’s 测试:患者抵抗手腕伸展,RMT在外上髁处检查疼痛反应。
- Mill’s 测试:患者伸直肘部并向下弯曲手腕,RMT观察外侧肘部疼痛情况。
- Maudsley’s 测试:患者抵抗中指伸展,检查外上髁疼痛。
- 握力测试:评估握物时的无力或不适。
What RMTs Can Do
RMT可以运用多种技术来缓解网球肘症状并促进康复,包括:
- 摩擦按摩:分解肌腱中的粘连和疤痕组织,改善血液循环,促进愈合。
- 触发点疗法:针对前臂肌肉的紧张区域,释放紧张并减轻疼痛。
- 筋膜松解:缓解包裹肌肉和肌腱的筋膜紧张,促进活动能力。
- 伸展与强化练习:温和的伸展和特定强化练习可以提高灵活性并减少肌腱压力。
- 瑞典式按摩:促进全身放松和循环,帮助减轻炎症和疼痛。
- 关节松动:松动周围结构以增强肘部的活动能力和功能。
Prevention
预防网球肘的关键在于减少前臂肌肉和肌腱的压力:
- 正确的技术:确保运动和工作中的动作正确,避免过度负担。
- 强化练习:加强前臂和手腕肌肉,提高耐受重复性动作的能力。
- 伸展练习:定期拉伸前臂肌肉,保持灵活性,防止紧张。
- 人体工学调整:调整工作环境或设备以减少肘部肌腱的压力。
- 休息:在高强度或重复性活动后给予前臂和肘部充分恢复时间,以防止过度使用。
通过合理的护理和预防策略,网球肘可以得到有效管理,减少疼痛并防止长期损伤。

網球肘,外上髁炎
網球肘,又稱外上髁炎,是指肘部外側的肌腱發炎,導致疼痛和無力。雖然名稱來自於網球運動,但這種狀況並不限於網球選手,任何反覆過度使用前臂肌肉的人都有可能患上。以下是其主要特徵的詳細說明:
Causes
網球肘是由於反覆的壓力和過度使用前臂肌肉,導致連接於外上髁(肘部外側)的肌腱出現微小撕裂。常見的原因包括:
- 反覆的手臂動作:如打網球、刷油漆、打字和使用工具等活動,會對前臂肌肉和肌腱施加壓力。
- 不正確的技術:在網球等運動中,或在涉及抓握和扭轉動作的活動中,使用不正確的技術或設備會增加對肘部肌腱的負擔。
- 年齡:網球肘多見於30至50歲之間,隨著年齡增長,肌腱變得不再那麼有彈性,且更容易受傷。
Symptoms
網球肘的主要症狀是肘部外側的疼痛,其他可能的症狀包括:
- 疼痛或灼熱感:從肘部外側延伸至前臂,特別是在抓握、提物或扭轉時感到疼痛。
- 無力:前臂力量減弱,抓握或提物變得困難。
- 壓痛感:肘部外側對觸摸敏感。
- 僵硬:早上或休息後肘部活動困難,無法完全伸直。
Special Tests RMTs Can Use
RMT可使用以下測試來評估網球肘:
- Cozen’s 測試:患者抵抗手腕伸展,RMT在外上髁處觸診,檢查是否有肌腱疼痛。
- Mill’s 測試:患者伸直肘部並向下彎曲手腕,RMT檢查外側肘部的疼痛情況。
- Maudsley’s 測試:患者對抗阻力伸展中指,檢查外上髁的疼痛。
- 握力測試:評估患者在握握物體時的無力或不適感。
What RMTs Can Do
RMT可使用多種技術來緩解網球肘的症狀並促進康復,包括:
- 摩擦按摩:分解肌腱中的疤痕組織和粘連,促進血液循環和癒合。
- 觸發點療法:針對前臂肌肉中的緊繃點,釋放緊張並減輕疼痛。
- 筋膜釋放:減少覆蓋肌肉和肌腱的筋膜緊張,促進活動。
- 伸展和強化運動:通過溫和的伸展和特定的強化運動來提高靈活性並減少肌腱壓力。
- 瑞典式按摩:促進全身放鬆和血液循環,有助於減輕炎症和疼痛。
- 關節鬆動術:改善肘部周圍的活動範圍和功能,促進關節靈活性。
Prevention
預防網球肘涉及減少對前臂肌肉和肌腱的壓力:
- 正確技術:無論是在運動中還是工作時,確保動作的正確性,避免過度壓力。
- 強化運動:加強前臂和手腕肌肉的力量,以更好應對重複的動作。
- 伸展運動:定期伸展前臂肌肉,保持靈活性,預防緊繃。
- 人體工學調整:調整工作環境或運動設備,減少對肘部肌腱的壓力。
- 休息:在進行強烈或重複的活動後,讓肘部和前臂肌肉有足夠的休息時間,以防止過度使用。
透過適當的護理和預防策略,網球肘可以得到有效的管理,減少疼痛並防止肌腱長期損傷。

Causes
跟腱炎通常是由跟腱上的重复压力引起的微小撕裂,导致炎症和退化。常见的原因包括:
- 过度使用:跑步、跳跃或高冲击运动会对跟腱施加过大的应力,尤其是缺乏充分热身或身体准备时。
- 不合适的鞋子:缺少足够支撑或缓冲的鞋子会加重跟腱的负担。
- 活动量骤增:运动强度或持续时间突然增加,而没有逐渐适应,会导致跟腱炎症。
- 小腿肌肉紧张:小腿肌肉过度紧绷会增加对跟腱的压力,导致炎症。
- 扁平足或高足弓:足部结构异常会导致跟腱承受不均的应力,增加受伤的风险。
Symptoms
跟腱炎的主要症状包括:
- 疼痛:脚跟后方的酸痛或剧痛,特别是在运动时或运动后,晨起或休息后疼痛尤为明显。
- 压痛:按压跟腱时有明显的疼痛感,尤其是在特定部位。
- 僵硬:早上或长时间休息后,踝关节难以伸展。
- 肿胀:跟腱区域可能出现肿胀或变厚,提示炎症存在。
- 活动受限:行走或跑步时推脚的能力下降,踝关节伸展受限。
Special Tests RMTs Can Use
RMT 可通过以下测试评估跟腱炎:
- 汤普森测试(Thompson Test):患者趴卧,RMT 挤压小腿肌肉,如果脚无法正常移动,可能有跟腱撕裂。
- 触诊:沿跟腱的长度进行触诊,评估是否存在压痛、增厚或炎症区域。
- 踝背屈测试(Dorsiflexion Test):患者将脚背屈,RMT 检查活动范围和疼痛反应。
What RMTs Can Do
RMT 可采用多种技术减轻跟腱炎的症状并促进康复,包括:
- 摩擦按摩:分解肌腱中的瘢痕组织和粘连,促进血液循环并加速愈合。
- 触发点疗法:靶向小腿肌肉中的紧张区域,释放肌肉紧张,减轻疼痛。
- 筋膜松解:放松包裹肌肉的筋膜,增加灵活性,减少对跟腱的压力。
- 伸展与强化练习:温和的伸展和特定的强化练习,有助于提高小腿肌肉的柔韧性,减少肌腱压力。
- 瑞典式按摩:改善全身血液循环,帮助减少炎症和疼痛。
- 关节松动术:通过对踝关节周围结构的动员,改善关节活动度。
Prevention
预防跟腱炎的关键在于减少对跟腱的过度应力,方法包括:
- 合适的鞋子:选择有良好支撑和缓冲的鞋子,尤其是在运动时。
- 伸展练习:定期伸展小腿肌肉,保持柔韧性,减少肌腱紧张。
- 逐步增加活动量:缓慢增加运动强度和持续时间,避免突然增加对跟腱的压力。
- 强化训练:强化小腿和脚踝的肌肉,增加跟腱的承受力。
- 热身与放松:每次运动前充分热身,运动后进行冷身,降低受伤风险。
- 休息:在高强度或重复活动后,给予跟腱和小腿肌肉充分的休息时间,防止过度使用。

Causes
跟腱炎通常由跟腱上的重複壓力導致,進而引起發炎和退化。常見的原因包括:
- 過度使用:跑步、跳躍或高衝擊運動會對跟腱造成過度壓力,特別是如果缺乏充分的熱身或身體條件準備。
- 不合適的鞋子:缺乏足夠支撐或緩衝的鞋子會給跟腱帶來過大的壓力。
- 活動量突然增加:快速增加運動的強度或持續時間,而沒有逐漸提高身體的承受能力,會導致跟腱發炎。
- 小腿肌肉緊繃:緊繃或僵硬的小腿肌肉會增加跟腱的壓力,從而引發炎症。
- 扁平足或高足弓:足部結構異常會影響跟腱在運動中的壓力分佈,增加受傷的風險。
Symptoms
跟腱炎的主要症狀包括:
- 疼痛:腳跟後方的酸痛或劇痛,尤其是在運動過程中或之後。早晨或休息一段時間後疼痛會加重。
- 壓痛:按壓跟腱時有明顯的疼痛感,特別是跟腱的某些區域。
- 僵硬:早上或長時間休息後,腳或踝關節伸展困難。
- 腫脹:跟腱部位可見腫脹或變厚,表示發炎。
- 活動受限:在行走或跑步時推動腳掌的能力下降,踝關節伸展的範圍受限。
Special Tests RMTs Can Use
RMT 可以使用以下測試來評估跟腱炎:
- 湯普森測試(Thompson Test):病人面朝下躺著,RMT 擠壓小腿肌肉,如果腳無法正常移動,則可能存在跟腱損傷。
- 觸診:RMT 沿著跟腱的長度進行觸診,以確定是否有壓痛、腫脹或增厚的區域。
- 踝背屈測試(Dorsiflexion Test):病人將腳向上屈曲,RMT 會評估活動範圍並檢查在伸展過程中是否有疼痛。
What RMTs Can Do
RMT 可以使用多種技術來緩解跟腱炎的症狀並促進癒合,包括:
- 摩擦按摩:打破肌腱中的疤痕組織和粘連,促進血液循環並加速癒合。
- 觸痛點療法:針對小腿肌肉中的緊繃區域,減少跟腱的張力。
- 筋膜釋放:放鬆圍繞小腿肌肉的筋膜,促進靈活性並減少對跟腱的壓力。
- 伸展與強化運動:進行溫和的伸展與強化運動,幫助提高小腿肌肉和跟腱的靈活性和耐受性。
- 瑞典式按摩:促進放鬆和血液循環,有助於減輕炎症和疼痛。
- 關節活動度恢復:透過對周邊結構進行動員,幫助恢復踝關節的活動範圍和功能。
Prevention
預防跟腱炎需要減少對跟腱的壓力,方法包括:
- 適合的鞋子:穿戴提供良好支撐和緩衝的鞋子,尤其是在運動時。
- 伸展運動:經常伸展小腿肌肉以保持靈活性,減少對跟腱的張力。
- 逐漸增加活動量:逐步提高運動強度和持續時間,避免突然增加對跟腱的負荷。
- 強化運動:強化小腿和下肢肌肉,以支持跟腱並提高其耐受性。
- 熱身和冷身:每次運動前進行充分的熱身,運動後進行冷身,降低受傷風險。
- 休息:在重複或高強度活動後,給跟腱和小腿肌肉足夠的休息時間,防止過度使用損傷。

腕管综合征/CTS
腕管综合征(CTS) 是一种常见的情况,会导致手部和手臂的疼痛、麻木和刺痛。正中神经从前臂延伸至手掌,经过手腕的腕管时受到压迫,就会产生症状。腕管是位于手腕掌侧的狭窄通道,当通道变得狭窄时,会引发一系列不适症状。以下是其主要特征的详细说明:
Causes
腕管综合征通常由一系列因素引起,这些因素会对正中神经施加压力:
- 重复使用手部:进行需要重复手部或手腕动作的活动(如打字或使用工具),可能会刺激手腕的肌腱,导致肿胀,从而对正中神经施加压力。
- 手腕解剖结构:有些人天生腕管较小,容易患上CTS。手腕骨折或脱臼也会改变隧道内的空间。
- 医疗状况:糖尿病、类风湿性关节炎和甲状腺功能障碍等疾病会增加CTS的风险,因为这些状况会引起炎症或肿胀。
- 液体滞留:怀孕、更年期或其他引起液体滞留的情况会导致手腕肿胀,从而增加对正中神经的压力。
- 工作环境因素:需要长时间或用力弯曲手腕的工作,如装配线工作或重物搬运,与较高的CTS风险相关。
Symptoms
腕管综合征通常分为几个阶段发展:
- 早期阶段:患者可能会感到拇指、食指和中指出现刺痛、麻木或灼热感。症状通常在夜间发生。
- 中期阶段:随着病情加重,这些感觉变得更加频繁,可能在白天发生,尤其是在握持物体或进行某些活动时。
- 晚期阶段:手部可能出现无力感,使握物或进行精细操作变得困难。如果不及时治疗,拇指根部周围的肌肉可能会退化。
Special Tests RMTs Can Use
注册按摩治疗师(RMT)可以进行以下测试来评估腕管综合征:
- Phalen’s Test(法伦氏测试):患者将手背对在一起,手腕弯曲60秒。如果出现刺痛或麻木,表明正中神经受压。
- Tinel’s Sign(提内尔征象):治疗师轻敲手腕的腕管部位,正面的测试结果会在手指上产生刺痛感。
- Two-Point Discrimination(两点识别测试):评估皮肤对两个点的触觉识别能力。感觉丧失可能表明神经损伤。
- Durkan’s Test(腕管压力测试):治疗师直接在腕管处施加压力,检查是否会引发疼痛、麻木或刺痛。
What RMTs Can Do
RMT可以通过以下方法缓解腕管综合征的症状:
- 摩擦按摩:分解肌腱的黏连,促进循环,减少炎症。
- 筋膜松解:减轻前臂和手腕周围的筋膜紧张,缓解正中神经的压力。
- 伸展:针对前臂屈肌和伸肌的伸展有助于恢复灵活性,减少腕管的压迫。
- 触发点疗法:针对如桡侧屈腕肌和指屈肌等相关肌肉的触发点,缓解其紧张。
- 神经滑动运动:这些运动促进正中神经在腕管中的健康滑动,减少受困的风险。
- 关节松动术:轻柔的手腕关节松动有助于增加活动范围,改善手部和手腕的功能。
Prevention
预防腕管综合征需要减少手腕的压力并保持良好的手部姿势:
- 调整重复性活动:在进行需要重复手腕动作的活动(如打字或使用工具)时,应定期休息。
- 人体工学调整:进行活动时,确保手腕处于中立位置。比如打字时保持手腕平直,使用符合人体工学的工具以减少压力。
- 伸展与锻炼:定期进行手部和手腕的伸展运动,以保持灵活性,减少正中神经受压的风险。
- 管理潜在健康状况:妥善管理糖尿病、关节炎或甲状腺疾病等健康状况,可以降低CTS的风险。

腕隧道症候群/CTS
腕隧道症候群(CTS) 是一種常見的狀況,會導致手部和手臂疼痛、麻木及刺痛感。當正中神經從前臂延伸至手掌,經過手腕處的腕隧道時受到壓迫,便會引發症狀。腕隧道是位於手腕掌側的一個狹窄通道,當它變得過於狹窄時,可能會引發一系列不適症狀。以下是其主要特徵的詳細說明:
Causes
腕隧道症候群通常由一系列因素引起,這些因素會對正中神經施加壓力:
- 重複使用手部:進行需要重複手部或手腕動作的活動(如打字或使用工具),可能會刺激手腕的肌腱,導致腫脹,進而對正中神經施加壓力。
- 手腕解剖結構:有些人天生腕隧道較小,這會使他們更容易患上CTS。手腕骨折或脫臼也會改變隧道內的空間。
- 醫療狀況:糖尿病、類風濕性關節炎及甲狀腺功能障礙等疾病可能會增加CTS的風險,因為這些狀況會引起炎症或腫脹。
- 液體滯留:懷孕、更年期或其他引起液體滯留的情況,會導致手腕腫脹,進而增加對正中神經的壓力。
- 工作環境因素:需要長時間或用力彎曲手腕的工作,如裝配線工作或重物搬運,與較高的CTS風險相關。
Symptoms
腕隧道症候群通常分階段發展:
- 早期階段:患者可能感覺拇指、食指和中指出現刺痛、麻木或灼熱感。症狀通常在夜間發生。
- 中期階段:隨著病情惡化,這些感覺變得更加頻繁,並且可能在白天發生,特別是在握持物體或進行某些活動時。
- 晚期階段:手部可能出現無力感,使握物或進行精細操作變得困難。如果不及時治療,拇指根部周圍的肌肉可能會退化。
Special Tests RMTs Can Use
註冊按摩治療師(RMT)可以進行以下測試來評估腕隧道症候群:
- Phalen’s Test(法倫氏測試):患者將手背對在一起,手腕彎曲60秒。如果出現刺痛或麻木,表明正中神經受壓。
- Tinel’s Sign(提內爾徵象):治療師輕敲手腕處的腕隧道,正面的測試結果會在手指上產生刺痛感。
- Two-Point Discrimination(兩點識別測試):評估皮膚能夠區分兩點觸碰的能力。感覺喪失可能表明神經損傷。
- Durkan’s Test(腕隧道壓力測試):治療師直接在腕隧道上施加壓力,檢查是否會引發疼痛、麻木或刺痛。
What RMTs Can Do
RMT可以通過以下方法來緩解腕隧道症候群的症狀:
- 摩擦按摩:分解肌腱的黏連,促進循環,減少炎症。
- 筋膜放鬆:減少前臂和手腕周圍的筋膜緊張,緩解對正中神經的壓力。
- 伸展:針對前臂屈肌和伸肌的伸展,有助於恢復靈活性,減少對腕隧道的壓迫。
- 觸發點療法:針對如橈側屈腕肌及指屈肌等相關肌肉的觸痛點,釋放其緊張。
- 神經滑動運動:這些運動促進正中神經在腕隧道中的健康運動,減少其受困的風險。
- 關節動員:輕柔的手腕關節動員可以增加活動範圍,改善手部和手腕的功能。
Prevention
預防腕隧道症候群需要減少手腕的壓力並保持良好的手部姿勢:
- 修改重複活動:在進行需要重複手腕動作的活動(如打字或使用工具)時,應定期休息。
- 人體工學調整:在進行活動時,確保手腕處於中立位置。比如打字時保持手腕平直,使用符合人體工學的工具來減少壓力。
- 伸展與運動:定期進行手部和手腕的伸展運動,以保持靈活性,減少正中神經受壓的風險。
- 管理潛在健康狀況:妥善管理糖尿病、關節炎或甲狀腺疾病等健康狀況,可降低CTS的風險。

狄奎凡氏综合症/狄奎凡氏腱鞘炎
狄奎凡氏综合症,又称狄奎凡氏腱鞘炎,是指拇指侧手腕的肌腱发炎,导致疼痛和不适。此症常见于从事重复性手部和手腕动作的人群,如提物、抓握或扭动手腕。以下是其主要方面的详细说明:
Causes
狄奎凡氏综合症是由于拇长外展肌腱和短伸肌腱在手腕附近受到刺激和发炎引起的。常见原因包括:
- 重复性手腕和拇指动作:如打字、发短信、编织和演奏乐器等活动可能会对肌腱造成压力。
- 过度使用:频繁提重物,特别是拇指和手腕处于不自然位置时,会导致肌腱发炎。
- 外伤:手腕或肌腱的直接创伤或损伤可能引发炎症。
- 怀孕及激素变化:怀孕期间的体液滞留及激素变化会增加罹患狄奎凡氏综合症的风险。
Symptoms
狄奎凡氏综合症的主要症状是拇指基部及手腕处的疼痛,可能还包括:
- 疼痛:当拇指或手腕移动时,特别是抓握或扭转动作时,疼痛加剧。
- 肿胀:拇指基部肿胀,可能形成可见的硬块。
- 拇指活动受限:拇指或手腕活动困难,特别是在抓握或捏合时。
- 触痛:拇指侧手腕对触摸特别敏感。
- 摩擦感:在移动肌腱时,可能感到摩擦或“吱吱”声。
Special Tests RMTs Can Use
RMT可以使用以下测试评估狄奎凡氏综合症:
- 芬克尔斯坦测试:患者将拇指放在手掌中握拳,然后将手腕向小指方向弯曲,若拇指侧手腕出现疼痛,则为狄奎凡氏综合症的阳性结果。
- 埃霍夫测试:与芬克尔斯坦测试相似,但由RMT被动进行,以检查肌腱疼痛。
- 触痛检查:RMT按压拇指基部肌腱,检查是否有压痛和肿胀。
What RMTs Can Do
RMT可以使用多种技术来减轻症状并促进康复,包括:
- 摩擦按摩:分解肌腱中的粘连和瘢痕组织,改善血液循环,减轻炎症。
- 触发点疗法:针对前臂和手部肌肉中的紧张区域,释放压力并减少疼痛。
- 筋膜松解:针对包裹肌肉和肌腱的筋膜,改善柔韧性并减少限制。
- 拇指及手腕伸展:轻柔的伸展动作,改善拇指和手腕的活动范围。
- 增强练习:强化拇指和前臂肌肉的练习,促进肌腱稳定性。
- 瑞典式按摩:促进全身血液循环,有助于减轻炎症和疼痛。
- 关节松动:通过松动周围结构来增强手腕和拇指关节的活动范围和功能。
Prevention
预防狄奎凡氏综合症的关键是减少手腕和拇指肌腱的压力:
- 人体工学:调整工作站或工具,减少手腕的重复性压力。
- 正确技术:在提物、抓握或打字等活动中保持手部和手腕正确姿势,减少肘部的压力。
- 增强锻炼:强化手部、手腕及前臂的肌肉,为肌腱提供更好的支持。
- 伸展:定期拉伸手腕和拇指肌肉,保持柔韧性,防止紧绷。
- 休息:在进行重复性活动后,给手腕和前臂肌肉足够的恢复时间,以防止过度使用伤害。
通过适当的护理和预防措施,狄奎凡氏综合症可以得到有效管理,减少疼痛并促进肌腱的长期健康。

狄奎凡氏症候群/狄奎凡氏腱鞘炎
狄奎凡氏症候群,又稱狄奎凡氏腱鞘炎,是指位於手腕拇指側的肌腱發炎,導致疼痛和不適。此症常見於從事重複性手部和手腕動作的人群,例如提物、抓握或扭動手腕。以下是其主要方面的詳細說明:
Causes
狄奎凡氏症候群是由位於手腕附近的拇長外展肌腱和短伸肌腱的刺激和發炎引起。常見原因包括:
- 重複性手腕和拇指動作:如打字、發簡訊、編織和演奏樂器等活動可能會對肌腱造成壓力。
- 過度使用:頻繁提重物,特別是拇指和手腕處於不自然位置時,會導致肌腱發炎。
- 外傷:手腕或肌腱的直接創傷或損傷可能引發炎症。
- 懷孕及荷爾蒙變化:懷孕期間的體液滯留及荷爾蒙變化會增加罹患狄奎凡氏症候群的風險。
Symptoms
狄奎凡氏症候群的主要症狀是在拇指基部及手腕處的疼痛,還可能包括:
- 疼痛:當拇指或手腕移動時,特別是抓握或扭轉動作時,疼痛會加劇。
- 腫脹:拇指基部腫脹,可能會形成可見的硬塊。
- 拇指活動受限:拇指或手腕活動困難,特別是在抓握或捏合時。
- 觸痛:拇指側的手腕對觸摸特別敏感。
- 摩擦感:在移動肌腱時,可能會感覺到磨擦或「吱吱」聲。
Special Tests RMTs Can Use
RMT可以使用以下測試來評估狄奎凡氏症候群:
- 芬克爾斯坦測試:患者將拇指放在手掌中握拳,然後將手腕向小指方向彎曲,若拇指側手腕出現疼痛,則為狄奎凡氏症候群的陽性結果。
- 埃霍夫測試:與芬克爾斯坦測試相似,但由RMT被動進行,以檢查肌腱疼痛。
- 觸痛檢查:RMT按壓拇指基部肌腱,檢查是否有壓痛和腫脹。
What RMTs Can Do
RMT可以應用多種技術來減輕症狀並促進康復,包括:
- 摩擦按摩:分解肌腱中的粘連和瘢痕組織,改善血液循環,減輕炎症。
- 觸發點療法:針對前臂和手部肌肉中的緊張區域,釋放壓力並減少疼痛。
- 筋膜釋放:針對包裹肌肉和肌腱的筋膜,改善柔韌性並減少限制。
- 拇指及手腕伸展:輕柔的伸展動作,改善拇指和手腕的活動範圍。
- 增強練習:強化拇指和前臂肌肉的練習,以促進肌腱穩定性。
- 瑞典式按摩:促進全身血液循環,有助於減少炎症和疼痛。
- 關節松動:通過松動周圍結構來增強手腕和拇指關節的活動範圍和功能。
Prevention
預防狄奎凡氏症候群的關鍵是減少手腕和拇指肌腱的壓力:
- 人體工學:調整工作站或工具,減少手腕的重複性壓力。
- 正確技術:在提物、抓握或打字等活動中保持手部和手腕正確的姿勢,減少肘部的壓力。
- 增強鍛煉:強化手部、手腕及前臂的肌肉,為肌腱提供更好的支撐。
- 伸展:定期拉伸手腕和拇指肌肉,保持柔韌性,防止緊繃。
- 休息:在進行重複性活動後,讓手腕和前臂肌肉有足夠的恢復時間,以防止過度使用傷害。
透過適當的護理和預防措施,狄奎凡氏症候群可得到有效管理,減少疼痛並促進肌腱的長期健康。

肩周炎
肩周炎,又称为黏连性肩关节囊炎,是一种肩膀疼痛僵硬并导致无法活动的情况。通常从逐渐加重的疼痛开始,限制肩部的活动。随着时间的推移,肩关节可能完全“冻结”,使日常活动变得困难。如果不进行治疗,这种情况可能会持续数年,且完全康复可能会被延迟或无法达成。以下是其主要特征的详细说明:
Causes
肩周炎的确切原因尚未完全了解,但有几个因素通常与其发展相关:
- 受伤或手术:肩部受伤或手术常会导致活动能力减少,从而使肩膀僵硬。
- 医疗状况:糖尿病、甲状腺疾病、心血管疾病以及帕金森病等都已知会增加肩周炎的风险。
- 活动受限:由于受伤、疾病或手术导致的长期不活动,可能会引发肩周炎。
- FOOSH(手臂伸直时跌倒):跌倒后,肩部旋转肌肉可能出现保护性痉挛,导致长期收缩,并严重限制肩部活动。如果这种情况持续,可能导致关节囊变化并发展为肩周炎。
Symptoms
肩周炎通常分为三个阶段发展:
- 冻结期:疼痛逐渐加剧,肩部活动变得受限。此阶段通常持续6周到9个月。
- 冻结期:疼痛可能减轻,但僵硬和活动受限变得更加明显,使日常任务变得困难。这个阶段可持续4到12个月。
- 解冻期:肩部活动逐渐改善,通常持续6个月到2年。然而,如果没有适当治疗,完全康复可能无法达成,且长期活动受限可能持续。
Special Tests RMTs Can Use
- AROM(主动活动范围测试):评估关节活动能力及旋转肌群的收缩功能品质。
- PROM(被动活动范围测试):评估肩关节的韧带和关节囊完整性。
- Empty Can Test(空罐测试):检查肩胛上肌是否参与疼痛。
- Hawkins Test(霍金斯测试):帮助排除或确认肩胛上肌肌腱的撞击问题。
- Painful Arc Test(疼痛弧测试):确认三角肌与肩胛上肌之间的弱点,并检查潜在的撞击问题。
- Scapular Rhythm Test(肩胛节奏测试):评估肩外展过程中上斜方肌的补偿情况。
What RMTs Can Do
- 摩擦:分解肌纤维以促进循环并增加活动范围。
- 关节动员:促进已减少或失去活动范围的关节恢复活动。
- 关节囊伸展:减少由关节囊黏连引起的关节囊限制。
- 针压与伸展:拉长内外旋肌以增强肩部旋转范围。
- 触发点释放:通过释放压痛点来减少肌肉紧张。
- 瑞典式按摩:改善整体循环,有助于减轻夜间疼痛。

肩周炎
肩周炎,又稱為黏連性肩關節囊炎,是一種肩膀疼痛僵硬並導致無法活動的狀況。通常從逐漸加重的疼痛開始,限制肩部的活動。隨著時間的推移,肩關節可能完全“凍結”,使日常活動變得困難。若不進行治療,該狀況可能會持續數年,且完全康復可能會被延遲或無法達成。以下是其主要特徵的詳細說明:
Causes
肩周炎的確切原因尚未完全了解,但有幾個因素通常與其發展相關:
- 受傷或手術:肩部受傷或手術常會導致活動能力減少,從而使肩膀僵硬。
- 醫療狀況:糖尿病、甲狀腺疾病、心血管疾病以及帕金森氏症等都已知會增加肩周炎的風險。
- 活動受限:由於受傷、疾病或手術導致的長期不活動,可能會引發肩周炎。
- FOOSH(手臂伸直時跌倒):跌倒後,肩部旋轉肌肉可能出現保護性痙攣,導致長期收縮,並嚴重限制肩部活動。如果這種情況持續,可能導致關節囊變化並發展為肩周炎。
Symptoms
肩周炎通常分為三個階段發展:
- 凍結期:疼痛逐漸加劇,肩部活動變得受限。此階段通常持續6週到9個月。
- 凍結期:疼痛可能減輕,但僵硬和活動受限變得更加明顯,使日常任務變得困難。這個階段可持續4到12個月。
- 解凍期:肩部活動逐漸改善,通常持續6個月到2年。然而,若無適當治療,完全康復可能無法達成,且長期活動受限可能持續。
Special Tests RMTs Can Use
- AROM(主動活動範圍測試):評估關節活動能力及旋轉肌群的收縮功能品質。
- PROM(被動活動範圍測試):評估肩關節的韌帶和關節囊完整性。
- Empty Can Test(空罐測試):檢查肩胛上肌是否參與疼痛。
- Hawkins Test(霍金斯測試):幫助排除或確認肩胛上肌肌腱的撞擊問題。
- Painful Arc Test(疼痛弧測試):確認三角肌與肩胛上肌之間的弱點,並檢查潛在的撞擊問題。
- Scapular Rhythm Test(肩胛節奏測試):評估肩外展過程中上斜方肌的補償情況。
What RMTs Can Do
- 摩擦:分解肌纖維以促進循環並增加活動範圍。
- 關節動員:促進已減少或失去活動範圍的關節恢復活動。
- 關節囊伸展:減少由關節囊黏連引起的關節囊限制。
- 針壓與伸展:拉長內外旋肌以增強肩部旋轉範圍。
- 觸發點釋放:通過釋放壓痛點來減少肌肉緊張。
- 瑞典式按摩:改善整體循環,有助於減輕夜間疼痛。

一般压力
一般压力 是人们面对日常生活中的压力和需求时的自然反应。适度的压力不一定有害,甚至能激发行动力和专注力。然而,长期的压力可能会导致身心健康问题,进而影响整体的生活质量。以下是关于一般压力的详细解说:
Causes
一般压力可能源于多种因素,包括:
- 工作压力:工作中的高需求、紧迫的截止日期或同事间的冲突,常常会引发持续的压力。
- 生活变化:如搬家、开始新工作或人际关系的变动,都可能触发压力。
- 财务问题:面对财务困境、债务压力或工作不稳定等问题时,容易产生压力。
- 健康问题:个人健康状况不佳,或照顾生病的亲人,可能带来巨大的情绪和心理压力。
- 过度承诺:过多的责任和事务,且缺乏足够的休息时间,会让人感到不堪重负。
Symptoms
压力的症状多种多样,常见的包括:
- 身体症状:头痛、肌肉紧绷、疲劳、胸痛或消化问题。
- 心理症状:难以集中注意力、思绪纷飞或感到难以应对。
- 情绪症状:焦虑、易怒、情绪波动或感到持续紧张。
- 行为症状:睡眠问题、过度饮食或食欲不振、社交退缩,或依赖酒精、咖啡因等来应对压力。
Special Tests RMTs Can Use
虽然压力本身无法通过具体的检查来诊断,但 RMT 可以通过观察以下状况来评估与压力相关的肌肉紧绷及不适:
- 姿势评估:识别压力常引发的肩颈和上背部紧张。
- 肌肉触诊:触摸检查特定肌肉群的紧绷感,尤其是下颌、背部和肩膀部位,这些部位常因压力而紧绷。
- 活动范围检查:检查是否有颈部或背部的活动受限,这可能表明因压力引发的肌肉僵硬。
What RMTs Can Do
RMT 可以运用多种按摩技术来缓解压力和放松身心,包括:
- 瑞典式按摩:促进全身放松并增加血液循环,帮助减少压力和肌肉紧张。
- 触发点疗法:针对因长期压力而紧绷的肌肉,释放压力点以减轻疼痛。
- 筋膜松解:轻柔拉伸包裹肌肉的筋膜,减少僵硬并提升灵活性。
- 芳香疗法按摩:使用如薰衣草或桉树等精油,在治疗过程中增强放松效果。
- 深层组织按摩:针对因长期压力积累的深层肌肉紧张进行治疗。
Prevention
预防和管理压力需要采取积极的步骤来维持身心健康平衡:
- 时间管理:计划并优先处理任务,以避免因责任过多而感到不堪重负。
- 定期运动:体育活动有助于释放积压的压力,促进放松感。
- 放松技巧:如深呼吸、冥想或瑜伽等练习,有助于减少压力并促进放松。
- 健康饮食:吃均衡的饮食,有助于稳定能量水平并改善情绪。
- 社交支持:与朋友或家人共度时光,有助于减少孤立感和压力。
- 良好的睡眠习惯:保持规律的作息时间并建立舒缓的睡前例行,减少压力并改善整体健康。
通过适当的管理技巧和支持,压力可以得到有效缓解,帮助人们维持更佳的身心健康。

一般壓力
一般壓力 是人們面對日常生活中的壓力和需求時的自然反應。適度的壓力不一定有害,甚至能激發行動力和專注力。然而,長期的壓力可能會導致身心健康問題,進而影響整體的生活品質。以下是關於一般壓力的詳細解說:
Causes
一般壓力可能源於多種因素,包括:
- 工作壓力:工作中的高需求、緊迫的截止日期或同事間的衝突,常常會引發持續的壓力。
- 生活變化:如搬家、開始新工作或人際關係的變動,都可能觸發壓力。
- 財務問題:面對財務困境、債務壓力或工作不穩定等問題時,容易產生壓力。
- 健康問題:個人健康狀況不佳,或照顧生病的親人,可能帶來巨大的情緒和心理壓力。
- 過度承諾:過多的責任和事務,且缺乏足夠的休息時間,會讓人感到不堪重負。
Symptoms
壓力的症狀多種多樣,常見的包括:
- 身體症狀:頭痛、肌肉緊繃、疲勞、胸痛或消化問題。
- 心理症狀:難以集中注意力、思緒紛飛或感到難以應對。
- 情緒症狀:焦慮、易怒、情緒波動或感到持續緊繃。
- 行為症狀:睡眠問題、過度飲食或食慾不振、社交退縮,或依賴酒精、咖啡因等來應對壓力。
Special Tests RMTs Can Use
雖然壓力本身無法通過具體的檢查來診斷,但 RMT 可以通過觀察以下狀況來評估與壓力相關的肌肉緊繃及不適:
- 姿勢評估:識別壓力常引發的肩頸和上背部緊張。
- 肌肉觸診:觸摸檢查特定肌肉群的緊繃感,尤其是下頜、背部和肩膀部位,這些部位常因壓力而緊繃。
- 活動範圍檢查:檢查是否有頸部或背部的活動受限,這可能表明因壓力引發的肌肉僵硬。
What RMTs Can Do
RMT 可以運用多種按摩技術來緩解壓力和放鬆身心,包括:
- 瑞典式按摩:促進全身放鬆並增加血液循環,幫助減少壓力和肌肉緊張。
- 觸發點療法:針對因長期壓力而緊繃的肌肉,釋放壓力點以減輕疼痛。
- 筋膜鬆解:輕柔拉伸包裹肌肉的筋膜,減少僵硬並提升靈活性。
- 芳香療法按摩:使用如薰衣草或桉樹等精油,在治療過程中增強放鬆效果。
- 深層組織按摩:針對因長期壓力累積的深層肌肉緊張進行治療。
Prevention
預防和管理壓力需要採取積極的步驟來維持身心健康平衡:
- 時間管理:計劃並優先處理任務,以避免因責任過多而感到不堪重負。
- 定期運動:體育活動有助於釋放積壓的壓力,促進放鬆感。
- 放鬆技巧:如深呼吸、冥想或瑜伽等練習,有助於減少壓力並促進放鬆。
- 健康飲食:吃均衡的飲食,有助於穩定能量水平並改善情緒。
- 社交支持:與朋友或家人共度時光,有助於減少孤立感和壓力。
- 良好的睡眠習慣:保持規律的作息時間並建立舒緩的睡前例行,減少壓力並改善整體健康。
透過適當的管理技巧和支持,壓力可以得到有效緩解,幫助人們維持更佳的身心健康。

Causes
高尔夫球肘是由前臂肌肉的重复性压力和过度使用引起的,导致附着在内上髁(肘部内侧)的肌腱出现小撕裂。常见原因包括:
- 重复的手臂动作:高尔夫球、投掷、抓握和使用手工具等活动会给前臂肌肉和肌腱带来压力。
- 不正确的技术:在高尔夫、球拍运动或举重等活动中,不正确的姿势会加重肘部肌腱的负担。
- 年龄:高尔夫球肘在40岁及以上的人群中更为常见,因为随着年龄的增长,肌腱的柔韧性下降,更容易受伤。
Symptoms
高尔夫球肘的主要症状是肘部内侧疼痛,但也可能包括:
- 疼痛或压痛:不适从肘部内侧向前臂延伸,特别是在抓握、提举或手腕弯曲时加剧。
- 无力:前臂力量减弱,使握住物体或提起物品变得困难。
- 僵硬:特别是在早晨或休息后,难以完全弯曲或伸直肘部。
- 麻木或刺痛感:感觉可能辐射到手指,特别是无名指和小指。
Special Tests RMTs Can Use
RMT可以使用以下测试来评估高尔夫球肘:
- 抗阻手腕屈曲测试:患者抵抗手腕屈曲,RMT在内上髁处触诊,检查是否有疼痛。
- 内上髁触诊:RMT按压肘部内侧,检测肌腱的压痛感。
- 高尔夫球肘测试:患者伸直肘部时,RMT屈曲手腕和手指,以评估内肘部的疼痛情况。
What RMTs Can Do
RMT可以应用多种技术来缓解高尔夫球肘症状并促进康复,包括:
- 摩擦按摩:分解肌腱中的粘连和疤痕组织,改善血液循环,帮助愈合。
- 触发点疗法:针对前臂肌肉中的紧张区域,释放紧张并减轻疼痛。
- 筋膜释放:释放包裹肌肉和肌腱的筋膜中的紧张,改善柔韧性和活动能力。
- 伸展和增强练习:温和的练习能增加肌腱的柔韧性并强化肌肉,减少压力。
- 瑞典式按摩:促进全身血液循环,有助于减少炎症和疼痛。
- 关节松动:通过松动周围结构来恢复肘关节的活动范围并改善其功能。
Prevention
预防高尔夫球肘的关键是减少前臂肌肉和肌腱的压力:
- 正确的技术:在运动或工作相关的重复手臂动作中,确保姿势正确,以减少肘部的压力。
- 增强练习:强化前臂肌肉以更好地应对重复动作。
- 伸展:定期拉伸前臂肌肉,保持柔韧性,防止紧张。
- 人体工学:调整工具、设备或工作站以减少对肘部肌腱的压力。
- 休息:在重复或高强度活动后,给肘部和前臂肌肉足够的恢复时间,以防止过度使用伤害。
通过适当的护理和预防措施,可以有效管理高尔夫球肘,减少疼痛并防止肌腱的长期损伤。

Causes
高爾夫球肘是由前臂肌肉的重複性壓力和過度使用引起的,導致附著在內上髁(肘部內側)的肌腱出現小撕裂。常見原因包括:
- 重複的手臂動作:高爾夫球、投擲、抓握和使用手工具等活動會給前臂肌肉和肌腱帶來壓力。
- 不正確的技術:在高爾夫、球拍運動或舉重等活動中,不正確的姿勢會加重肘部肌腱的負擔。
- 年齡:高爾夫球肘在40歲及以上的人群中更為常見,因為隨著年齡的增長,肌腱的柔韌性下降,更容易受傷。
Symptoms
高爾夫球肘的主要症狀是肘部內側疼痛,但也可能包括:
- 疼痛或壓痛:不適從肘部內側向前臂延伸,特別是在抓握、提舉或手腕彎曲時加劇。
- 無力:前臂力量減弱,使握住物體或提起物品變得困難。
- 僵硬:特別是在早晨或休息後,難以完全彎曲或伸直肘部。
- 麻木或刺痛感:感覺可能輻射到手指,特別是無名指和小指。
Special Tests RMTs Can Use
RMT可以使用以下測試來評估高爾夫球肘:
- 抗阻手腕屈曲測試:患者抵抗手腕屈曲,RMT在內上髁處觸診,檢查是否有疼痛。
- 內上髁觸診:RMT按壓肘部內側,檢測肌腱的壓痛感。
- 高爾夫球肘測試:患者伸直肘部時,RMT屈曲手腕和手指,以評估內肘部的疼痛情況。
What RMTs Can Do
RMT可以應用多種技術來緩解高爾夫球肘症狀並促進康復,包括:
- 摩擦按摩:分解肌腱中的粘連和疤痕組織,改善血液循環,幫助愈合。
- 觸發點療法:針對前臂肌肉中的緊張區域,釋放緊張並減輕疼痛。
- 筋膜釋放:釋放包裹肌肉和肌腱的筋膜中的緊張,改善柔韌性和活動能力。
- 伸展和增強練習:溫和的練習能增加肌腱的柔韌性並強化肌肉,減少壓力。
- 瑞典式按摩:促進全身血液循環,有助於減少炎症和疼痛。
- 關節松動:通過松動周圍結構來恢復肘關節的活動範圍並改善其功能。
Prevention
預防高爾夫球肘的關鍵是減少前臂肌肉和肌腱的壓力:
- 正確的技術:在運動或工作相關的重複手臂動作中,確保姿勢正確,以減少肘部的壓力。
- 增強練習:強化前臂肌肉以更好地應對重複動作。
- 伸展:定期拉伸前臂肌肉,保持柔韌性,防止緊張。
- 人體工學:調整工具、設備或工作站以減少對肘部肌腱的壓力。
- 休息:在重複或高強度活動後,給肘部和前臂肌肉足夠的恢復時間,以防止過度使用傷害。
通過適當的護理和預防措施,可以有效管理高爾夫球肘,減少疼痛並防止肌腱的長期損傷。
下背痛
下背痛是常见的健康问题,影响各年龄层和不同生活方式的人。它可能源自不良姿势、肌肉拉伤或受伤,表现为刺痛、钝痛或放射性疼痛。根据原因,下背痛可为急性或慢性,有时会影响日常活动和整体活动能力。以下是其主要特征的详细说明:
Causes
下背痛的常见原因包括:
- 肌肉拉伤或扭伤:由于抬重物、突然动作或运动时姿势不当造成的肌肉或韧带拉伤,可能引发下背痛。
- 不良姿势:长时间坐着或站立姿势不正确会对下背部施加压力,导致疼痛和不适。
- 退行性疾病:骨关节炎、退化性椎间盘病或椎间盘突出可导致脊柱关节和椎间盘的磨损,造成慢性下背痛。
- 受伤或创伤:跌倒、事故或运动损伤会损害下背部的脊柱、肌肉或韧带。
- 坐骨神经痛:由椎间盘突出压迫坐骨神经,导致疼痛从下背部延伸至腿部。
Symptoms
下背痛可根据其原因以不同形式表现:
- 局部疼痛:疼痛集中于下背部,可能表现为刺痛或钝痛。
- 放射性疼痛:疼痛延伸至一条或两条腿(坐骨神经痛),有时伴随麻木或刺痛感。
- 僵硬感:活动范围受限,弯腰或扭转时困难。
- 肌肉痉挛:突然且痛苦的肌肉收缩,限制活动能力。
- 无力或麻木:若涉及神经,可能会感到腿部无力或麻木。
Special Tests RMTs Can Use
RMT可使用以下测试来评估下背痛:
- 活动范围测试(ROM):评估脊柱的灵活性并确定紧张或不适的区域。
- 直腿抬高测试:通过抬高直腿来评估是否有坐骨神经痛或神经根压迫。
- 触诊:轻轻按压特定区域,以识别肌肉痉挛、压痛或紧绷。
- Patrick’s(FABER)测试:检查髋关节是否有问题,这有时也会导致下背痛。
- Slump测试:评估神经张力,常用于诊断坐骨神经痛。
What RMTs Can Do
RMT可使用多种技术来缓解下背痛并恢复功能:
- 深层组织按摩:针对深层肌肉组织,释放慢性紧张并减轻疼痛。
- 触发点疗法:针对紧张肌肉中的特定点,缓解放射性疼痛并改善灵活性。
- 筋膜释放:通过拉伸结缔组织来改善活动范围并减少疼痛。
- 瑞典式按摩:温和的技术能促进血液循环,减少肌肉紧张并促进放松。
- 关节松动术:恢复僵硬或受限关节的活动能力,增强整体活动范围。
- 伸展和强化运动:RMT可能会推荐一些运动来加强核心肌肉,帮助支撑下背部并预防未来疼痛。
Prevention
预防下背痛需要保持健康的生活方式,并注意身体姿势和运动方式:
- 良好姿势:在坐、站和抬重物时保持脊柱的正确对齐,以减少对下背部的压力。
- 定期运动:通过平板支撑、桥式等运动来加强支撑脊柱的核心肌肉。
- 正确抬物技巧:始终用腿来抬重物,避免扭转脊柱。
- 伸展运动:定期伸展腿筋、臀部和下背部,保持灵活性并减少僵硬感。
- 人体工学调整:确保工作环境和睡眠环境支持良好的姿势和脊柱对齐。
通过适当的护理、预防策略和治疗,下背痛可以得到有效管理,从而改善生活质量并预防复发。

下背痛
下背痛是常見的健康問題,影響各年齡層和不同生活方式的人。它可能源自不良姿勢、肌肉拉傷或受傷,表現為刺痛、鈍痛或放射性疼痛。根據原因,下背痛可為急性或慢性,有時會影響日常活動和整體活動能力。以下是其主要特徵的詳細說明:
Causes
下背痛的常見原因包括:
- 肌肉拉傷或扭傷:由於抬重物、突然動作或運動時姿勢不當造成的肌肉或韌帶拉傷,可能引發下背痛。
- 不良姿勢:長時間坐著或站立姿勢不正確會對下背部施加壓力,導致疼痛和不適。
- 退行性疾病:骨關節炎、退化性椎間盤病或椎間盤突出可導致脊柱關節和椎間盤的磨損,造成慢性下背痛。
- 受傷或創傷:跌倒、事故或運動損傷會損害下背部的脊柱、肌肉或韌帶。
- 坐骨神經痛:由椎間盤突出壓迫坐骨神經,導致疼痛從下背部延伸至腿部。
Symptoms
下背痛可根據其原因以不同形式表現:
- 局部疼痛:疼痛集中於下背部,可能表現為刺痛或鈍痛。
- 放射性疼痛:疼痛延伸至一條或兩條腿(坐骨神經痛),有時伴隨麻木或刺痛感。
- 僵硬感:活動範圍受限,彎腰或扭轉時困難。
- 肌肉痙攣:突然且痛苦的肌肉收縮,限制活動能力。
- 無力或麻木:若涉及神經,可能會感到腿部無力或麻木。
Special Tests RMTs Can Use
RMT可使用以下測試來評估下背痛:
- 活動範圍測試(ROM):評估脊柱的靈活性並確定緊張或不適的區域。
- 直腿抬高測試:通過抬高直腿來評估是否有坐骨神經痛或神經根壓迫。
- 觸診:輕輕按壓特定區域,以識別肌肉痙攣、壓痛或緊繃。
- Patrick’s(FABER)測試:檢查髖關節是否有問題,這有時也會導致下背痛。
- Slump測試:評估神經張力,常用於診斷坐骨神經痛。
What RMTs Can Do
RMT可使用多種技術來緩解下背痛並恢復功能:
- 深層組織按摩:針對深層肌肉組織,釋放慢性緊張並減輕疼痛。
- 觸發點療法:針對緊張肌肉中的特定點,緩解放射性疼痛並改善靈活性。
- 筋膜釋放:通過拉伸結締組織來改善活動範圍並減少疼痛。
- 瑞典式按摩:溫和的技術能促進血液循環,減少肌肉緊張並促進放鬆。
- 關節鬆動術:恢復僵硬或受限關節的活動能力,增強整體活動範圍。
- 伸展和強化運動:RMT可能會推薦一些運動來加強核心肌肉,幫助支撐下背部並預防未來疼痛。
Prevention
預防下背痛需要保持健康的生活方式,並注意身體姿勢和運動方式:
- 良好姿勢:在坐、站和抬重物時保持脊椎的正確對齊,以減少對下背部的壓力。
- 定期運動:通過平板支撐、橋式等運動來加強支撐脊柱的核心肌肉。
- 正確抬物技巧:始終用腿來抬重物,避免扭轉脊柱。
- 伸展運動:定期伸展腿筋、臀部和下背部,保持靈活性並減少僵硬感。
- 人體工學調整:確保工作環境和睡眠環境支持良好的姿勢和脊柱對齊。
通過適當的護理、預防策略和治療,下背痛可以得到有效管理,從而改善生活質量並預防復發。

足底筋膜炎
足底筋膜炎 是一种常见疾病,指的是足底筋膜(一条沿着脚底的厚组织带)发炎。该发炎会导致脚跟疼痛,尤其在行走或站立时,使活动变得困难。疼痛通常在早晨或长时间静止后最为严重。如果不及时治疗,足底筋膜炎可能会持续数月甚至数年,严重影响日常生活。以下是对其关键方面的详细解释:
Causes
多种因素可能导致足底筋膜炎的发生,包括:
- 过度使用或过量活动: 反复的压力,如跑步、跳舞或长时间站立,会对足底筋膜造成拉扯。
- 足部力学问题: 高足弓、扁平足或异常的步态都可能增加足底筋膜的负担。
- 不适合的鞋子: 缺乏支撑力的鞋子,尤其是鞋底薄或缺乏足弓支撑的鞋子,可能加剧足底筋膜炎的发展。
- 肥胖: 体重过重会增加足底筋膜的压力,导致发炎。
- 小腿肌肉或跟腱紧绷: 这些部位的柔韧性下降会对足底筋膜产生牵拉,增加受伤风险。
Symptoms
足底筋膜炎通常表现出以下症状:
- 脚跟疼痛: 特别是在早晨或静止后的第一步,脚跟会出现尖锐的刺痛感。
- 运动后疼痛: 虽然在活动期间疼痛可能减轻,但在运动后或长时间站立后疼痛会加重。
- 僵硬与触痛: 尤其是沿着足弓和脚跟部位,脚可能感觉紧绷或触摸时感到疼痛。
Special Tests RMTs Can Use
为了评估足底筋膜炎,注册按摩治疗师 (RMT) 可能会进行以下测试:
- Windlass Test (足底筋膜张力测试): 通过将大脚趾上翘来检测足底筋膜的张力,观察是否出现疼痛或紧绷感。
- 触诊: 通过按压足底筋膜来确定疼痛和发炎的区域。
- 步态分析: 观察患者的行走方式,找出可能导致足底筋膜炎的足部力学问题。
- 踝关节背屈测试: 评估小腿肌肉和跟腱的柔韧性,这些区域的紧绷可能影响足底筋膜的张力。
What RMTs Can Do
RMT 可以使用多种技术来减轻疼痛、减少发炎并促进足底筋膜的康复:
- 深层组织按摩: 针对足底筋膜和周围肌肉,释放紧张并改善血液循环。
- 筋膜松动术: 针对筋膜的粘连进行释放,改善活动范围。
- 触发点疗法: 释放小腿肌肉中的紧张点,减少足底筋膜的张力。
- 交叉摩擦按摩: 帮助分解疤痕组织,促进足底筋膜的愈合。
- 伸展技术: 着重于拉伸小腿肌肉和跟腱,减少对足底筋膜的压力。
- 足部和踝关节松动术: 改善足部和踝关节的活动范围,减少对足底筋膜的压力。
Prevention
预防足底筋膜炎的关键在于解决其根本原因,并保持足部和腿部肌肉的柔韧性与力量。主要的预防策略包括:
- 穿着有支撑力的鞋子: 带有良好足弓支撑和缓冲鞋底的鞋子有助于减少足底筋膜的压力。
- 伸展: 定期拉伸小腿肌肉和跟腱可以减少足底筋膜的张力。
- 强化运动: 强化足部和踝关节的肌肉,可以改善足部力学,减少足底筋膜的压力。
- 保持健康体重: 减少过多的体重可以减轻对脚的压力。
- 避免过度使用: 逐渐增加运动强度,并在需要时休息,可以防止因过度使用而导致的足底筋膜炎。

足底筋膜炎
足底筋膜炎 是一種常見的疾病,指的是足底筋膜(沿著腳底的一條厚組織帶)發炎。這種發炎會導致腳跟疼痛,特別是在行走或站立時,會使活動變得困難。疼痛通常在早晨或長時間靜止後最為嚴重。如果不及時治療,足底筋膜炎可能會持續數月甚至數年,嚴重影響日常生活。以下是對其關鍵方面的詳細解釋:
Causes
多種因素可能導致足底筋膜炎的發生,包括:
- 過度使用或過量活動: 反覆的壓力,如跑步、跳舞或長時間站立,會對足底筋膜造成拉扯。
- 足部力學問題: 高足弓、扁平足或異常的步態都可能增加足底筋膜的負擔。
- 不適合的鞋子: 缺乏支撐力的鞋子,尤其是鞋底薄或缺乏足弓支撐的鞋子,會加劇足底筋膜炎的發展。
- 肥胖: 體重過重會增加足底筋膜的壓力,導致發炎。
- 小腿肌肉或跟腱緊繃: 這些部位的柔韌性下降會對足底筋膜產生牽拉,增加受傷風險。
Symptoms
足底筋膜炎通常表現出以下症狀:
- 腳跟疼痛: 特別是在早晨或靜止後的第一步,腳跟會出現尖銳的刺痛感。
- 運動後疼痛: 雖然在活動期間疼痛可能減輕,但在運動後或長時間站立後疼痛會加重。
- 僵硬與觸痛: 尤其是沿著足弓和腳跟部位,腳可能感覺緊繃或觸摸時感到疼痛。
Special Tests RMTs Can Use
為了評估足底筋膜炎,註冊按摩治療師 (RMT) 可能會進行以下測試:
- Windlass Test (足底筋膜張力測試): 通過將大腳趾上翹來檢測足底筋膜的張力,觀察是否出現疼痛或緊繃感。
- 觸診: 通過按壓足底筋膜來確定疼痛和發炎的區域。
- 步態分析: 觀察患者的行走方式,找出可能導致足底筋膜炎的足部力學問題。
- 踝關節背屈測試: 評估小腿肌肉和跟腱的柔韌性,這些區域的緊繃可能影響足底筋膜的張力。
What RMTs Can Do
RMT 可以使用多種技術來減輕疼痛、減少發炎並促進足底筋膜的康復:
- 深層組織按摩: 針對足底筋膜和周圍肌肉,釋放緊張並改善血液循環。
- 筋膜鬆動術: 針對筋膜的粘連進行釋放,改善活動範圍。
- 觸發點療法: 釋放小腿肌肉中的緊張點,減少足底筋膜的張力。
- 交叉摩擦按摩: 幫助分解疤痕組織,促進足底筋膜的癒合。
- 伸展技術: 著重於拉伸小腿肌肉和跟腱,減少對足底筋膜的壓力。
- 足部和踝關節鬆動術: 改善足部和踝關節的活動範圍,減少對足底筋膜的壓力。
Prevention
預防足底筋膜炎的關鍵在於解決其根本原因,並保持足部和腿部肌肉的柔韌性與力量。主要的預防策略包括:
- 穿著有支撐力的鞋子: 帶有良好足弓支撐和緩衝鞋底的鞋子有助於減少足底筋膜的壓力。
- 伸展: 定期拉伸小腿肌肉和跟腱可以減少足底筋膜的張力。
- 強化運動: 強化足部和踝關節的肌肉,可以改善足部力學,減少足底筋膜的壓力。
- 保持健康體重: 減少過多的體重可以減輕對腳的壓力。
- 避免過度使用: 逐漸增加運動強度,並在需要時休息,可以防止因過度使用而導致的足底筋膜炎。

肩部撞击综合症
肩部撞击综合症 是指肩部的肌腱或滑囊在活动时被压迫或刺激,导致疼痛和活动受限。此症状常见于运动员以及从事重复性高举动作的人群。如果不及时治疗,肩部撞击可能会逐渐恶化,进而导致更严重的问题,如肌腱撕裂。以下是其关键方面的详细解释:
Causes
肩部撞击综合症的常见原因包括:
- 重复性高举动作: 如游泳、网球和举重等活动,可能导致肩部肌腱摩擦周围组织,产生炎症和刺激。
- 肩部肌肉无力或不平衡: 旋转袖肌群力量不足或肩部肌肉不平衡,会破坏肩部正常的活动功能,增加撞击风险。
- 不良姿势: 前倾的头部或圆肩姿势会改变肩胛骨的位置,导致肩部撞击的可能性增加。
- 年龄相关的磨损: 随着年龄的增长,肩部的肌腱和滑囊可能会退化,使肩部撞击的风险上升。
- 骨刺: 肩关节的异常骨增生会减少肌腱的活动空间,导致撞击发生。
Symptoms
肩部撞击综合症通常表现为以下症状:
- 高举动作时疼痛: 当手臂举过肩膀时,尤其是做伸展或高举动作时,肩部会出现疼痛。
- 肩部无力: 可能会感受到肩部力量下降,导致无法轻松举起或搬运物体。
- 僵硬和活动受限: 肩部可能感觉僵硬或紧绷,特别是在长时间静止后。
- 夜间疼痛: 肩部撞击的患者通常在夜间躺卧于患侧时,疼痛加重,影响睡眠质量。
Special Tests RMTs Can Use
为了评估肩部撞击综合症,注册按摩治疗师 (RMT) 可能会进行以下测试:
- Neer’s Test: 治疗师被动抬起患者手臂,同时稳定肩胛骨,观察是否有疼痛感,判断是否存在撞击。
- Hawkins-Kennedy Test: 治疗师将患者的肩膀和肘部弯曲至90度,然后内旋手臂,检查是否有疼痛,可能提示冈上肌撞击。
- Painful Arc Test: 测试患者在肩部外展60到120度时是否出现疼痛,这可能意味着撞击存在。
- Empty Can Test: 通过让患者在“拇指朝下”的姿势下抵抗向下的压力,检查冈上肌的无力或疼痛。
- Speed’s Test: 该测试检查肱二头肌腱是否有疼痛,因为它也可能与肩部撞击综合症有关。
What RMTs Can Do
RMT 可以使用多种技术来减轻疼痛、恢复肩部活动能力并预防进一步损伤:
- 触发点释放: 针对旋转袖肌群及其周围的紧张点,缓解疼痛并改善肌肉功能。
- 深层组织按摩: 作用于肩部的深层肌肉,释放紧张,促进血液循环,加快愈合。
- 筋膜松动术: 专注于肩部肌肉周围的筋膜,打破粘连,增加活动范围。
- 关节松动术: 温和地活动肩关节,恢复正常活动,减少对肌腱的压迫。
- 伸展: 改善肩部和胸部肌肉的柔韧性,减轻紧张并改善姿势。
- 强化训练: 帮助强化旋转袖肌群和肩胛稳定肌肉,纠正肌肉不平衡,预防未来的撞击问题。
Prevention
预防肩部撞击的关键在于保持肩部肌肉的强壮和柔韧,并保持良好的姿势和正确的活动模式。主要预防措施包括:
- 加强旋转袖肌群: 定期锻炼以加强旋转袖肌群,有助于保持正常的肩部活动机制,减少撞击风险。
- 改善姿势: 维持良好的姿势,特别是在上背部和肩部,可以避免肩部结构受到压迫。
- 避免重复性高举动作: 限制或调整涉及重复性高举动作的活动,减少肩部压力。
- 伸展肩部和胸部肌肉: 定期进行拉伸,可以改善肩部柔韧性,减少紧张,促进更好的活动模式。
- 正确的技术: 无论是运动还是日常活动,确保在高举动作中使用正确的技术,防止肩部承受不必要的压力。

肩部夾擊綜合症
肩部夾擊綜合症 是指肩部的肌腱或滑囊在活動時被壓迫或刺激,導致疼痛和活動受限。這種情況常見於運動員和經常從事重複性高舉動作的人群。如果不及時治療,肩部夾擊可能會隨著時間惡化,進而引發更嚴重的問題,如肌腱撕裂。以下是其關鍵方面的詳細說明:
Causes
多種因素可能導致肩部夾擊綜合症的發生,包括:
- 重複性的高舉動作: 如游泳、網球和舉重等活動,會使肩部的肌腱摩擦周圍結構,導致刺激和炎症。
- 肩部肌肉力量不足或不平衡: 旋轉袖肌群的弱化或肩部力量的不平衡,會破壞肩部的正常機械功能,增加夾擊風險。
- 不良姿勢: 頭部前傾或圓肩姿勢會改變肩胛骨的位置,增加夾擊的可能性。
- 年齡相關的磨損: 隨著年齡增長,肩部的肌腱和滑囊可能會退化,使得夾擊更加容易發生。
- 骨刺: 肩關節的異常骨增生會減少肌腱的活動空間,導致夾擊。
Symptoms
肩部夾擊綜合症通常表現出以下症狀:
- 高舉動作時疼痛: 在肩部高度以上抬手時,尤其是伸手或舉過頭頂時會出現疼痛。
- 肩部無力: 可能會明顯感覺到肩部力量下降,導致舉物或搬運物品變得困難。
- 僵硬與活動範圍受限: 肩部可能感覺僵硬,尤其是在長時間不活動後。
- 夜間疼痛: 許多肩部夾擊患者在躺在患側肩部時,疼痛會加劇,影響睡眠。
Special Tests RMTs Can Use
為了評估肩部夾擊綜合症,註冊按摩治療師 (RMT) 可能會進行以下測試:
- Neer’s Test: 治療師在固定肩胛骨的情況下,被動抬起患者的手臂,檢查是否有疼痛,以判斷是否存在夾擊。
- Hawkins-Kennedy Test: 治療師將患者的肩膀和肘部彎曲至90度,然後內旋手臂,檢查是否有疼痛,這可能表明岡上肌夾擊。
- Painful Arc Test: 測試患者在肩部外展的60至120度之間是否出現疼痛,這通常表明存在夾擊。
- Empty Can Test: 通過讓患者在“拇指朝下”的姿勢下抵抗向下壓力,檢查岡上肌的無力或疼痛。
- Speed’s Test: 這項測試檢查肱二頭肌腱是否有疼痛,因為它也可能涉及肩部夾擊綜合症。
What RMTs Can Do
RMT 可以採用多種技術來減輕疼痛,恢復肩部的活動能力,並防止進一步損傷:
- 觸發點釋放: 針對旋轉袖肌群和周圍區域的緊張點,緩解疼痛並改善肌肉功能。
- 深層組織按摩: 針對肩部的深層肌肉進行按摩,釋放緊繃並促進血液循環,加速恢復。
- 筋膜鬆動術: 集中處理肩部肌肉周圍的筋膜,打破粘連,增加活動範圍。
- 關節鬆動術: 輕柔地活動肩關節,恢復正常運動,減少對肌腱的壓迫。
- 伸展: 著重於改善肩部和胸部肌肉的柔韌性,減輕緊張,改善姿勢。
- 強化運動: 幫助強化旋轉袖肌群和肩胛穩定肌肉,糾正肌肉不平衡,防止未來的夾擊發生。
Prevention
預防肩部夾擊的關鍵在於保持肩部肌肉的強壯和柔韌,以及採用正確的姿勢和運動模式。主要的預防策略包括:
- 強化旋轉袖肌群: 定期進行強化旋轉袖肌群的運動,有助於保持正常的肩部機械功能,降低夾擊風險。
- 改善姿勢: 維持良好的姿勢,特別是在上背部和肩部,可以防止肩部結構被壓迫。
- 避免重複的高舉動作: 限制或調整涉及重複性高舉動作的活動,減少對肩部的壓力。
- 拉伸肩部和胸部肌肉: 定期進行拉伸可以改善柔韌性,減少肩部和周圍肌肉的緊張,促進更好的活動模式。
- 採用正確技術: 無論是運動還是日常活動,確保在高舉動作中使用正確的技術,防止肩部承受不必要的壓力。

紧张性头痛
紧张性头痛 是一种常见的头痛类型,通常表现为头部两侧的压迫感或紧绷感。它可能由多种因素引起,包括压力、肌肉紧张和不良的生活习惯。虽然紧张性头痛通常不是严重的健康问题,但频繁发作可能会影响日常生活和工作。以下是关于紧张性头痛的详细解说:
Causes
紧张性头痛的主要原因包括:
- 肌肉紧张:长时间保持不良姿势,特别是在办公桌前,容易导致颈部和肩部肌肉紧张,进而引发头痛。
- 心理压力:工作、家庭或生活中的压力和焦虑可能导致肌肉紧张,诱发头痛。
- 缺乏休息:长时间工作而没有休息,尤其是在精神高度集中的情况下,可能引起紧张性头痛。
- 眼睛疲劳:长时间注视电脑屏幕或手机,容易导致眼部疲劳和紧张,从而引发头痛。
- 脱水:水分不足可能导致身体不适,包括头痛。
Symptoms
紧张性头痛的症状通常包括:
- 头部紧绷感:感觉头部像被束缚一样,有压迫感。
- 钝痛:头痛通常是轻到中等的钝痛,通常不伴随恶心或呕吐。
- 颈部和肩部紧张:伴随颈部和肩部的肌肉紧绷和不适。
- 疲劳感:可能会感到身体疲惫,精神集中困难。
Special Tests RMTs Can Use
虽然紧张性头痛无法通过具体的检查来诊断,但 RMT 可以通过以下方法来评估与头痛相关的肌肉紧张和不适:
- 姿势评估:检查患者的坐姿和站姿,识别是否有不良姿势导致的肌肉紧张。
- 肌肉触诊:触摸颈部、肩部和头部肌肉,评估是否有压痛或紧绷感。
- 活动范围检查:检查颈部活动范围是否受限,了解肌肉的紧张程度。
What RMTs Can Do
RMT 可以采用多种按摩技术来缓解紧张性头痛的症状,包括:
- 瑞典式按摩:通过轻柔的手法放松全身肌肉,缓解紧张感,改善血液循环。
- 深层组织按摩:针对颈部和肩部的深层肌肉紧张,帮助释放紧绷的肌肉。
- 头部按摩:轻柔按摩头部、太阳穴和后颈部,以减轻头痛。
- 触发点疗法:针对特定的紧张点,释放肌肉紧张和疼痛。
- 放松技巧:结合深呼吸、冥想等放松技巧,帮助缓解心理压力。
Prevention
预防紧张性头痛需要采取一些积极的措施:
- 保持良好姿势:确保在工作时坐姿正确,避免长时间保持同一姿势。
- 定期休息:每工作一段时间就休息几分钟,站起来活动一下,缓解肌肉紧张。
- 管理压力:通过运动、冥想或其他放松技巧来管理心理压力。
- 保持水分:确保每天摄入足够的水分,避免脱水。
- 眼睛休息:使用电脑或手机时,每隔一段时间看向远处,缓解眼睛疲劳。
通过适当的管理和治疗,紧张性头痛可以得到有效缓解,改善生活质量。

緊張性頭痛
緊張性頭痛 是一種常見的頭痛類型,通常表現為頭部兩側的壓迫感或緊繃感。它可能由多種因素引起,包括壓力、肌肉緊張和不良的生活習慣。雖然緊張性頭痛通常不是嚴重的健康問題,但頻繁發作可能會影響日常生活和工作。以下是關於緊張性頭痛的詳細解說:
Causes
緊張性頭痛的主要原因包括:
- 肌肉緊張:長時間保持不良姿勢,特別是在辦公桌前,容易導致頸部和肩部肌肉緊張,進而引發頭痛。
- 心理壓力:工作、家庭或生活中的壓力和焦慮可能導致肌肉緊張,誘發頭痛。
- 缺乏休息:長時間工作而沒有休息,尤其是在精神高度集中的情況下,可能引起緊張性頭痛。
- 眼睛疲勞:長時間注視電腦螢幕或手機,容易導致眼部疲勞和緊張,從而引發頭痛。
- 脫水:水分不足可能導致身體不適,包括頭痛。
Symptoms
緊張性頭痛的症狀通常包括:
- 頭部緊繃感:感覺頭部像被束縛一樣,有壓迫感。
- 鈍痛:頭痛通常是輕到中等的鈍痛,通常不伴隨噁心或嘔吐。
- 頸部和肩部緊張:伴隨頸部和肩部的肌肉緊繃和不適。
- 疲勞感:可能會感到身體疲憊,精神集中困難。
Special Tests RMTs Can Use
雖然緊張性頭痛無法通過具體的檢查來診斷,但 RMT 可以通過以下方法來評估與頭痛相關的肌肉緊張和不適:
- 姿勢評估:檢查患者的坐姿和站姿,識別是否有不良姿勢導致的肌肉緊張。
- 肌肉觸診:觸摸頸部、肩部和頭部肌肉,評估是否有壓痛或緊繃感。
- 活動範圍檢查:檢查頸部活動範圍是否受限,了解肌肉的緊張程度。
What RMTs Can Do
RMT 可以採用多種按摩技術來緩解緊張性頭痛的症狀,包括:
- 瑞典式按摩:通過輕柔的手法放鬆全身肌肉,緩解緊張感,改善血液循環。
- 深層組織按摩:針對頸部和肩部的深層肌肉緊張,幫助釋放緊繃的肌肉。
- 頭部按摩:輕柔按摩頭部、太陽穴和後頸部,以減輕頭痛。
- 觸發點療法:針對特定的緊張點,釋放肌肉緊張和疼痛。
- 放鬆技巧:結合深呼吸、冥想等放鬆技巧,幫助緩解心理壓力。
Prevention
預防緊張性頭痛需要採取一些積極的措施:
- 保持良好姿勢:確保在工作時坐姿正確,避免長時間保持同一姿勢。
- 定期休息:每工作一段時間就休息幾分鐘,站起來活動一下,緩解肌肉緊張。
- 管理壓力:通過運動、冥想或其他放鬆技巧來管理心理壓力。
- 保持水分:確保每天攝入足夠的水分,避免脫水。
- 眼睛休息:使用電腦或手機時,每隔一段時間看向遠處,緩解眼睛疲勞。
通過適當的管理和治療,緊張性頭痛可以得到有效緩解,改善生活質量。

颞下颌关节综合征
颞下颌关节综合征 是指下颌关节及周围肌肉的疼痛或功能障碍。这种情况可能会导致不适、咀嚼困难,以及下颌卡住或发出声音。TMJ 综合征可以影响任何年龄段的人,通常与压力、受伤或下颌错位有关。以下是关于 TMJ 综合征的详细解说:
Causes
TMJ 综合征可能由多种因素引发,包括:
- 下颌受伤:下颌或头部的创伤,如颈部鞭打伤或直接撞击,可能导致关节发炎或错位。
- 磨牙:睡眠时磨牙或咬紧牙齿会对下颌关节和肌肉造成过度压力。
- 关节炎:下颌关节的骨性关节炎或类风湿性关节炎会导致软骨退化,引起疼痛和僵硬。
- 压力:情绪压力会引起肌肉紧张,导致咬紧或紧张,进而引发 TMJ 综合征。
- 咬合不正:牙齿或下颌结构错位,会对 TMJ 施加不均的压力,增加不适。
Symptoms
TMJ 综合征的常见症状包括:
- 下颌疼痛:下颌、面部或耳朵周围的不适或酸痛,尤其是在咀嚼或说话时。
- 下颌卡住或发声:打开或闭合嘴巴时有明显的卡住、弹响或摩擦声。
- 活动受限:打开或闭合嘴巴的困难,严重时下颌可能卡住不动。
- 头痛:因咬紧牙齿引发的紧张型头痛或偏头痛。
- 耳痛或耳鸣:耳朵的疼痛或耳鸣,有时可能被误认为是耳部感染。
- 面部肿胀:颞下颌关节周围的压痛或肿胀,提示有炎症。
Special Tests RMTs Can Use
RMT 可通过以下测试评估 TMJ 综合征:
- 触诊测试:RMT 轻轻按压 TMJ 及周围肌肉,检查是否存在压痛或发炎。
- 活动范围测试:通过要求患者张口和闭口,检查下颌的活动范围是否有任何限制或偏离。
- 关节声音测试:RMT 观察下颌活动期间是否有弹响或摩擦声,以评估关节功能障碍。
- 咬合测试:患者咬合时,RMT 检查是否有疼痛或不适,以确认肌肉或关节问题。
What RMTs Can Do
RMT 可采用多种技术来缓解 TMJ 综合征的症状并改善下颌功能,包括:
- 触发点疗法:针对下颌、颈部和头部肌肉的紧绷区域进行释放,减少紧张和疼痛。
- 筋膜松解:放松包裹肌肉的筋膜,增加灵活性并减少不适。
- 口内按摩:在口腔内进行轻柔按摩,针对 TMJ 周围的肌肉,缓解紧张和不适。
- 颈肩按摩:放松颈部和上背部的肌肉,减少可能引发 TMJ 疼痛的紧张。
- 伸展练习:进行温和的下颌伸展练习,改善活动范围,减轻 TMJ 压力。
- 放松技术:通过按摩技术帮助管理压力,减少咬紧下颌的情况。
Prevention
预防 TMJ 综合征涉及管理压力并避免过度使用下颌的活动:
- 压力管理:练习深呼吸或冥想等放松技巧,减少压力,避免咬紧下颌。
- 避免硬食:限制硬或难嚼的食物,如口香糖或坚硬的肉类,以免加重 TMJ。
- 姿势意识:保持良好的姿势,尤其是在坐着或使用电子设备时,减少对颈部和下颌的压力。
- 夜间护齿器:佩戴夜间护齿器或夹板,防止磨牙,减轻 TMJ 压力。
- 下颌运动:进行温和的下颌伸展和强化练习,增强肌肉力量并提高灵活性。
- 避免过度下颌运动:避免过度使用下颌肌肉的活动,如嚼口香糖或咬指甲。
通过适当的护理和预防措施,TMJ 综合征可以得到有效管理,减轻疼痛并改善下颌功能。

顳顎關節症候群
顳顎關節症候群 是指顎關節及周圍肌肉的疼痛或功能障礙。此狀況可能導致不適、咀嚼困難,以及顎部卡住或發出聲音。TMJ 症候群可影響任何年齡層,通常與壓力、受傷或顎部錯位有關。以下是關於 TMJ 症候群的詳細解說:
Causes
TMJ 症候群可能由多種因素引發,包括:
- 顎部受傷:顎部或頭部的創傷,如頸部甩鞭傷或直接撞擊,可能導致關節發炎或錯位。
- 磨牙癖:睡眠時磨牙或咬緊牙齒,會對顎關節和肌肉造成過度壓力。
- 關節炎:顎關節的骨性關節炎或類風濕性關節炎會導致軟骨退化,引起疼痛和僵硬。
- 壓力:情緒壓力會引起肌肉緊繃,導致咬緊或緊張,進而引發 TMJ 症候群。
- 咬合不正:牙齒或顎部結構錯位,會對 TMJ 施加不均的壓力,增加不適。
Symptoms
TMJ 症候群的常見症狀包括:
- 顎部疼痛:顎部、臉部或耳朵周圍的不適或酸痛,尤其是在咀嚼或說話時。
- 顎部卡住或發聲:打開或閉合嘴巴時有明顯的卡住、彈響或摩擦聲。
- 活動受限:打開或閉合嘴巴的困難,嚴重時顎部可能卡住不動。
- 頭痛:因咬緊牙齒引發的緊張型頭痛或偏頭痛。
- 耳痛或耳鳴:耳朵的疼痛或耳鳴,有時可能被誤認為是耳部感染。
- 面部腫脹:顳顎關節周圍的壓痛或腫脹,提示有炎症。
Special Tests RMTs Can Use
RMT 可通過以下測試評估 TMJ 症候群:
- 觸診測試:RMT 輕輕按壓 TMJ 及周圍肌肉,檢查是否存在壓痛或發炎。
- 活動範圍測試:通過要求患者張口和閉口,檢查顎部的活動範圍是否有任何限制或偏離。
- 關節聲音測試:RMT 觀察顎部活動期間是否有彈響或摩擦聲,以評估關節功能障礙。
- 咬合測試:患者咬合時,RMT 檢查是否有疼痛或不適,以確認肌肉或關節問題。
What RMTs Can Do
RMT 可採用多種技術來緩解 TMJ 症候群的症狀並改善顎部功能,包括:
- 觸發點療法:針對顎部、頸部和頭部肌肉的緊繃區域進行釋放,減少緊張和疼痛。
- 筋膜松解:放鬆包裹肌肉的筋膜,增加靈活性並減少不適。
- 口內按摩:在口腔內進行輕柔按摩,針對 TMJ 周圍的肌肉,緩解緊張和不適。
- 頸肩按摩:放鬆頸部和上背部的肌肉,減少可能引發 TMJ 疼痛的緊張。
- 伸展練習:進行溫和的顎部伸展練習,改善活動範圍,減輕 TMJ 壓力。
- 放鬆技術:通過按摩技術幫助管理壓力,減少咬緊顎部的情況。
Prevention
預防 TMJ 症候群涉及管理壓力並避免過度使用顎部的活動:
- 壓力管理:練習深呼吸或冥想等放鬆技巧,減少壓力,避免咬緊顎部。
- 避免硬食:限制硬或難嚼的食物,如口香糖或堅硬的肉類,以免加重 TMJ。
- 姿勢意識:保持良好的姿勢,尤其是在坐著或使用電子設備時,減少對頸部和顎部的壓力。
- 夜間護齒器:佩戴夜間護齒器或夾板,防止磨牙,減輕 TMJ 壓力。
- 顎部運動:進行溫和的顎部伸展和強化練習,增強肌肉力量並提高靈活性。
- 避免過度顎部運動:避免過度使用顎部肌肉的活動,如嚼口香糖或咬指甲。
通過適當的護理和預防措施,TMJ 症候群可以得到有效管理,減輕疼痛並改善顎部功能。
頸部和上背部疼痛
頸部和上背部疼痛是現代生活中常見的問題,通常由於不良姿勢、過度使用或受傷引起。疼痛可能表現為肌肉緊繃、僵硬或刺痛,嚴重時可能影響日常活動。這種疼痛通常來自於肌肉、韌帶、神經或關節的勞損或過度使用。以下是其主要特徵的詳細說明:
Causes
頸部和上背部疼痛的常見原因包括:
- 不良姿勢:長時間坐著、駝背或低頭看手機、電腦,會導致頸部和上背部肌肉緊繃。
- 過度使用:反覆性的動作,如長時間打字、提重物或以不正確姿勢運動,會導致肌肉和關節受損。
- 受傷:如鞭打傷、突然衝擊或跌倒,會損傷頸部和上背部的肌肉、韌帶或關節。
- 壓力:情緒壓力會使頸部和上背部肌肉緊張,從而引發疼痛。
- 退行性病變:如骨關節炎或退化性椎間盤病,因關節和椎間盤磨損,會導致慢性頸部和上背部疼痛。
Symptoms
頸部和上背部疼痛的表現形式多種多樣:
- 肌肉僵硬:肌肉緊繃或痙攣,通常伴隨著活動範圍受限。
- 刺痛或鈍痛:疼痛可能局部集中,也可能向肩膀或手臂放射,影響日常活動。
- 頭痛:疼痛可能向上延伸至頭部,導致緊張型頭痛。
- 麻木或刺痛感:如果神經受到壓迫,可能會感到手臂或手部的麻木、刺痛或無力感。
Special Tests RMTs Can Use
RMT可通過以下測試來評估頸部和上背部疼痛:
- 活動範圍測試(ROM):包括主動和被動活動範圍測試,用來評估關節的靈活性及肌肉緊張情況。
- Spurling’s Test(斯伯林測試):通過在頭部傾斜時施加壓力,檢查是否有神經根壓迫。若測試陽性,可能表明頸椎神經病變。
- Upper Limb Tension Test(上肢張力測試):通過伸展手臂的神經,評估神經是否受張力影響。
- Cervical Compression and Distraction Tests(頸椎壓縮和牽引測試):用來判斷是否由神經壓迫或脊柱問題引起的疼痛。
What RMTs Can Do
RMT可通過多種技術來緩解頸部和上背部疼痛並改善活動能力:
- 觸發點釋放:針對肌肉中的結節進行釋放,減少肌肉緊張和疼痛。
- 筋膜釋放:通過拉伸筋膜來減少組織的限制,改善活動範圍並緩解疼痛。
- 瑞典式按摩:溫和的技術可增加血液循環,放鬆緊張的肌肉。
- 深層組織按摩:專注於深層肌肉組織,以釋放慢性緊張。
- 關節鬆動術:幫助恢復僵硬關節的活動能力,改善整體靈活性和功能。
- 姿勢教育:教導客戶如何在日常活動中保持正確姿勢,預防未來的疼痛。
Prevention
預防頸部和上背部疼痛需要保持良好的姿勢並調整日常活動:
- 人體工學調整:確保工作環境設置能保持脊椎的中立位置,特別是在長時間坐著時。
- 定期活動:在一天中定期起身活動、伸展,避免僵硬。
- 強化運動:加強支持頸部和上背部的肌肉(如斜方肌和菱形肌),預防肌肉不平衡。
- 壓力管理:通過深呼吸或冥想等放鬆技巧來減少壓力引起的肌肉緊張。
通過處理根本原因和症狀,適當的治療和預防策略可以有效管理頸部和上背部疼痛。

颈部和上背部疼痛
颈部和上背部疼痛是现代生活中常见的问题,通常由于不良姿势、过度使用或受伤引起。疼痛可能表现为肌肉紧绷、僵硬或刺痛,严重时可能影响日常活动。这种疼痛通常来自于肌肉、韧带、神经或关节的劳损或过度使用。以下是其主要特征的详细说明:
Causes
颈部和上背部疼痛的常见原因包括:
- 不良姿势:长时间坐着、驼背或低头看手机、电脑,会导致颈部和上背部肌肉紧绷。
- 过度使用:重复性的动作,如长时间打字、提重物或以不正确姿势运动,会导致肌肉和关节受损。
- 受伤:如鞭打伤、突然冲击或跌倒,会损伤颈部和上背部的肌肉、韧带或关节。
- 压力:情绪压力会使颈部和上背部肌肉紧张,从而引发疼痛。
- 退行性病变:如骨关节炎或退化性椎间盘病,因关节和椎间盘磨损,会导致慢性颈部和上背部疼痛。
Symptoms
颈部和上背部疼痛的表现形式多种多样:
- 肌肉僵硬:肌肉紧绷或痉挛,通常伴随着活动范围受限。
- 刺痛或钝痛:疼痛可能局部集中,也可能向肩膀或手臂放射,影响日常活动。
- 头痛:疼痛可能向上延伸至头部,导致紧张型头痛。
- 麻木或刺痛感:如果神经受到压迫,可能会感到手臂或手部的麻木、刺痛或无力感。
Special Tests RMTs Can Use
RMT可通过以下测试来评估颈部和上背部疼痛:
- 活动范围测试(ROM):包括主动和被动活动范围测试,用来评估关节的灵活性及肌肉紧张情况。
- Spurling’s Test(斯伯林测试):通过在头部倾斜时施加压力,检查是否有神经根压迫。若测试阳性,可能表明颈椎神经病变。
- Upper Limb Tension Test(上肢张力测试):通过伸展手臂的神经,评估神经是否受张力影响。
- Cervical Compression and Distraction Tests(颈椎压缩和牵引测试):用来判断是否由神经压迫或脊柱问题引起的疼痛。
What RMTs Can Do
RMT可通过多种技术来缓解颈部和上背部疼痛并改善活动能力:
- 触发点释放:针对肌肉中的结节进行释放,减少肌肉紧张和疼痛。
- 筋膜释放:通过拉伸筋膜来减少组织的限制,改善活动范围并缓解疼痛。
- 瑞典式按摩:温和的技术可增加血液循环,放松紧张的肌肉。
- 深层组织按摩:专注于深层肌肉组织,以释放慢性紧张。
- 关节松动术:帮助恢复僵硬关节的活动能力,改善整体灵活性和功能。
- 姿势教育:教导客户如何在日常活动中保持正确姿势,预防未来的疼痛。
Prevention
预防颈部和上背部疼痛需要保持良好的姿势并调整日常活动:
- 人体工学调整:确保工作环境设置能保持脊椎的中立位置,特别是在长时间坐着时。
- 定期活动:在一天中定期起身活动、伸展,避免僵硬。
- 强化运动:加强支持颈部和上背部的肌肉(如斜方肌和菱形肌),预防肌肉不平衡。
- 压力管理:通过深呼吸或冥想等放松技巧来减少压力引起的肌肉紧张。
通过处理根本原因和症状,适当的治疗和预防策略可以有效管理颈部和上背部疼痛。

Upper back and neck pain
Neck and upper back pain is a common issue in modern life, often caused by poor posture, overuse, or injury. It can present as muscle tension, stiffness, or sharp pain, and in severe cases, it may interfere with daily activities. The pain may stem from muscles, ligaments, nerves, or joints being strained or overused. Below is a detailed explanation of its key aspects:
Causes
Common causes of neck and upper back pain include:
– Poor posture: Prolonged sitting, slouching, or looking down at phones or computers can lead to tension in the neck and upper back muscles.
– Overuse: Repetitive motions or actions, such as typing for long hours, lifting heavy objects, or exercising with improper form, can strain the muscles and joints.
– Injury: Whiplash, sudden impacts, or falls can damage the muscles, ligaments, or joints in the neck and upper back.
– Stress: Emotional stress can cause muscle tightness, particularly in the neck and upper back region, contributing to pain.
– Degenerative conditions: Conditions like osteoarthritis or degenerative disc disease can cause chronic neck and upper back pain due to wear and tear on the joints and discs.
Symptoms
Neck and upper back pain can manifest in several ways:
1. Muscle stiffness: Tightness or spasms in the muscles, often accompanied by limited range of motion.
2. Sharp or aching pain: Pain may be localized or radiate to the shoulders or arms, making it difficult to perform daily tasks.
3. Headaches: Pain may travel up the neck and cause tension headaches.
4. Numbness or tingling: If nerves are compressed, you may experience numbness, tingling, or weakness in the arms or hands.
Special Tests RMTs Can Use
To assess neck and upper back pain, RMTs may use the following tests:
– Range of Motion (ROM): Both active and passive ROM tests are used to evaluate joint flexibility and muscle tension.
– Spurling’s Test: Checks for nerve root compression by applying pressure to the neck while the head is tilted. A positive test may indicate cervical radiculopathy.
– Upper Limb Tension Test (ULTT): Assesses nerve tension and involvement by stretching nerves in the arm.
– Cervical Compression and Distraction Tests: Used to determine if nerve compression or spinal issues are causing the pain.
What RMTs Can Do
RMTs can apply various techniques to relieve neck and upper back pain and improve mobility:
– Trigger Point Release: Targets knots in muscles to reduce tension and pain.
– Myofascial Release: Involves stretching the fascia to reduce restrictions in the tissue, improving range of motion and alleviating pain.
– Swedish Massage: Gentle techniques increase blood flow and relax tense muscles.
– Deep Tissue Massage: Focuses on deeper layers of muscle tissue to release chronic tension.
– Joint Mobilization: Helps to restore movement in stiff joints, improving overall flexibility and function.
– Postural Education: Teaching clients how to improve posture in daily activities to prevent future pain.
Prevention
Preventing neck and upper back pain involves maintaining good posture and making adjustments to daily activities:
– Ergonomic adjustments: Ensure that workspaces are set up to promote a neutral spine position, especially if you sit for long periods.
– Regular movement: Take breaks to stand, stretch, and move around during the day to avoid stiffness.
– Strengthening exercises: Strengthen the muscles that support the neck and upper back, such as the trapezius and rhomboids, to prevent muscle imbalances.
– Stress management: Practicing relaxation techniques like deep breathing or meditation can help reduce muscle tension caused by stress.
By addressing the underlying causes and symptoms, proper treatment and prevention strategies can effectively manage neck and upper back pain.

Temporomandibular Joint (TMJ) Syndrome
Temporomandibular Joint (TMJ) Syndrome refers to pain or dysfunction in the jaw joint and surrounding muscles. This condition can cause discomfort, difficulty in chewing, and jaw clicking or locking. TMJ syndrome can affect people of all ages and is often related to stress, injury, or jaw misalignment. Below is a detailed overview of TMJ syndrome:
Causes
TMJ syndrome can be triggered by several factors, including:
– Jaw Injury: Trauma to the jaw or head, such as whiplash or a direct hit, can cause inflammation or misalignment in the joint.
– Bruxism: Teeth grinding or clenching, especially during sleep, puts excessive strain on the jaw joint and muscles.
– Arthritis: Osteoarthritis or rheumatoid arthritis in the jaw joint can cause deterioration of the cartilage, leading to pain and stiffness.
– Stress: Emotional stress can cause muscle tension, leading to jaw clenching or tightening, which may result in TMJ syndrome.
– Misaligned Bite: Abnormal alignment of teeth or jaw structure can cause uneven pressure on the TMJ.
Symptoms
Common symptoms of TMJ syndrome include:
– Jaw Pain: Discomfort or aching in the jaw, face, or around the ear, especially when chewing or speaking.
– Jaw Clicking or Popping: Audible clicking, popping, or grating sounds when opening or closing the mouth.
– Limited Movement: Difficulty opening or closing the mouth fully, and in severe cases, the jaw may lock in place.
– Headaches: Tension headaches or migraines, often associated with jaw clenching.
– Earaches or Tinnitus: Pain or ringing in the ears, sometimes mistaken for an ear infection.
– Facial Swelling: Tenderness or swelling around the jaw joint.
Special Tests RMTs Can Use
RMTs may perform the following tests to assess TMJ syndrome:
– Palpation Test: RMTs gently press on the TMJ and surrounding muscles to assess for tenderness or inflammation.
– Range of Motion Test: Evaluates the jaw’s movement by asking the patient to open and close their mouth, checking for any limitations or deviations.
– Joint Sounds Test: RMT listens for clicking or popping sounds during jaw movement to assess joint dysfunction.
– Bite Test: The patient bites down while the RMT assesses for pain or discomfort, which may indicate muscle or joint involvement.
What RMTs Can Do
RMTs can use various techniques to relieve TMJ syndrome symptoms and improve jaw function, including:
– Trigger Point Therapy: Focuses on releasing tight areas in the jaw, neck, and head muscles to reduce tension and pain.
– Myofascial Release: Helps relieve tension in the fascia surrounding the muscles, promoting better mobility and reducing pain.
– Intraoral Massage: Gentle massage inside the mouth targeting the muscles around the TMJ to alleviate tightness and discomfort.
– Neck and Shoulder Massage: Reduces tension in the neck and upper back muscles that may contribute to TMJ pain.
– Stretching Exercises: Gentle stretches to improve the range of motion in the jaw and alleviate pressure on the TMJ.
– Relaxation Techniques: Massage techniques that help manage stress, reducing the likelihood of jaw clenching.
Prevention
Preventing TMJ syndrome involves managing stress and avoiding activities that overstrain the jaw:
– Stress Management: Practice relaxation techniques, such as deep breathing or meditation, to reduce stress and prevent jaw clenching.
– Avoid Hard Foods: Limit the consumption of hard or chewy foods, such as gum or tough meat, that can aggravate the TMJ.
– Posture Awareness: Maintain good posture, especially when sitting or using electronic devices, to reduce strain on the neck and jaw.
– Mouth Guards: Wearing a night guard or splint can help prevent teeth grinding and relieve pressure on the TMJ.
– Jaw Exercises: Perform gentle jaw stretches and exercises to strengthen the muscles and improve flexibility.
– Avoid Excessive Jaw Movements: Minimize activities like chewing gum or biting nails that overwork the jaw muscles.
With proper care and preventative measures, TMJ syndrome can be managed effectively, reducing pain and improving jaw function.

Tension Headache
Tension headache is a common type of headache that typically presents as a feeling of pressure or tightness around the head, often affecting both sides. It can be triggered by various factors, including stress, muscle tension, and poor lifestyle habits. While tension headaches are generally not a serious health issue, frequent episodes can impact daily life and productivity. Here’s a detailed explanation of its key aspects:
Causes
Tension headaches are primarily caused by:
– Muscle tension: Poor posture, especially when sitting at a desk for long periods, can lead to tightness in the neck and shoulder muscles, triggering headaches.
– Psychological stress: Stress and anxiety from work, family, or daily life can lead to muscle tension, which may cause headaches.
– Lack of rest: Prolonged periods of work without breaks, especially during mentally demanding tasks, can result in tension headaches.
– Eye strain: Extended periods of staring at computer screens or mobile devices can lead to fatigue and tension in the eyes, resulting in headaches.
– Dehydration: Insufficient fluid intake can cause discomfort, including headaches
Symptoms
The primary symptoms of tension headaches typically include:
– Tightness in the head: A sensation of pressure around the head, often described as feeling like a tight band.
– Dull pain: The headache is usually a mild to moderate dull ache, typically not accompanied by nausea or vomiting.
– Neck and shoulder tension: Accompanying muscle tightness and discomfort in the neck and shoulders.
– Fatigue: A feeling of tiredness and difficulty concentrating may occur.
Special Tests RMTs Can Use
While tension headaches cannot be diagnosed through specific tests, RMTs can assess muscle tension and discomfort associated with headaches through:
– Postural assessment: Evaluating the patient’s sitting and standing posture to identify any postural issues contributing to muscle tension.
– Muscle palpation: Assessing tenderness and tightness in the neck, shoulder, and head muscles.
– Range of motion checks: Evaluating neck movement to determine the level of muscle tightness and restrictions.
What RMTs Can Do
RMTs can apply various techniques to alleviate tension headache symptoms, including:
– Swedish massage: Using gentle strokes to promote overall relaxation and improve blood circulation, helping to relieve muscle tension.
– Deep tissue massage: Targeting deep layers of muscle tension in the neck and shoulders to help release tightness.
– Head massage: Gently massaging the head, temples, and back of the neck to reduce headache intensity.
– Trigger point therapy: Focusing on specific tight areas to release muscle tension and pain.
– Relaxation techniques: Incorporating deep breathing, meditation, or other relaxation practices to alleviate psychological stress.
Prevention
Preventing tension headaches involves taking proactive steps:
– Maintain good posture: Ensure proper sitting posture while working to avoid prolonged muscle strain.
– Take regular breaks: Pause every so often during work to stand, stretch, and relieve muscle tension.
– Manage stress: Utilize exercise, meditation, or other relaxation techniques to manage psychological stress.
– Stay hydrated: Drink sufficient water daily to avoid dehydration.
– Eye rest: Take breaks from screens to alleviate eye strain, looking away periodically to relax the eyes.
With appropriate management and treatment, tension headaches can be effectively alleviated, leading to improved quality of life.

Shoulder impingement syndromes
Shoulder impingement syndromes occur when the tendons or bursa in the shoulder become compressed or irritated during movement, leading to pain and limited mobility. This condition commonly affects athletes and individuals who engage in repetitive overhead activities. Without proper treatment, shoulder impingement can worsen over time, leading to more severe issues like tendon tears. Below is a detailed explanation of its key aspects:
Causes
Several factors can contribute to shoulder impingement syndromes, including:
– Repetitive overhead motions: Activities like swimming, tennis, and weightlifting can cause the tendons in the shoulder to rub against the surrounding structures, leading to irritation.
– Weak or imbalanced shoulder muscles: Weakness in the rotator cuff muscles or imbalances in shoulder strength can disrupt normal shoulder mechanics, increasing the risk of impingement.
– Poor posture: Forward head or rounded shoulder posture can alter the positioning of the shoulder blade, increasing the likelihood of impingement.
– Age-related wear and tear: Over time, the tendons and bursa in the shoulder may degenerate, making impingement more likely.
– Bone spurs: Abnormal bone growths in the shoulder joint can reduce the space available for tendons, leading to impingement.
Symptoms
Shoulder impingement syndromes typically present with the following symptoms:
1. Pain during overhead movements: Pain often occurs when lifting the arm above shoulder height, especially when reaching behind or overhead.
2. Shoulder weakness: There may be a noticeable decrease in shoulder strength, making it difficult to perform tasks like lifting or carrying objects.
3. Stiffness and limited range of motion: The shoulder may feel stiff or tight, particularly after periods of inactivity.
4. Pain at night: Many individuals with shoulder impingement experience increased discomfort while lying on the affected shoulder, disrupting sleep.
Special Tests RMTs Can Use
To assess shoulder impingement, a Registered Massage Therapist (RMT) may perform the following tests:
– Neer’s Test: The therapist passively raises the client’s arm while stabilizing the scapula to assess for pain, indicating possible impingement.
– Hawkins-Kennedy Test: The therapist flexes the shoulder and elbow to 90 degrees, then internally rotates the arm to check for pain, which can indicate supraspinatus impingement.
– Painful Arc Test: This test identifies pain occurring between 60-120 degrees of shoulder abduction, suggesting impingement.
– Empty Can Test: Assesses for weakness or pain in the supraspinatus muscle by having the client resist downward pressure with the arm in a “thumbs-down” position.
– Speed’s Test: This test checks for pain in the biceps tendon, which can also be involved in impingement syndromes.
What RMTs Can Do
RMTs can apply various techniques to reduce pain, restore mobility, and prevent further damage in clients with shoulder impingement:
– Trigger Point Release: Targets tension in the rotator cuff muscles and surrounding areas to relieve pain and improve muscle function.
– Deep Tissue Massage: Works on the deeper muscles of the shoulder to release tightness and improve circulation, promoting healing.
– Myofascial Release: Focuses on the fascia surrounding the shoulder muscles to break down adhesions and increase mobility.
– Joint Mobilization: Gently mobilizes the shoulder joint to restore proper movement and reduce compression on the tendons.
– Stretching: Focuses on improving flexibility in the shoulder and chest muscles to relieve tension and improve posture.
– Strengthening Exercises: Assists in strengthening the rotator cuff and scapular stabilizers to correct muscle imbalances and prevent future impingement.
Prevention
Preventing shoulder impingement involves maintaining strong and flexible shoulder muscles, as well as adopting proper posture and movement patterns. Key prevention strategies include:
– Strengthening the rotator cuff: Regular exercises to strengthen the rotator cuff muscles can help maintain proper shoulder mechanics and reduce the risk of impingement.
– Improving posture: Maintaining good posture, especially in the upper back and shoulders, can help prevent compression of the shoulder structures.
– Avoiding repetitive overhead activities: Limiting or modifying activities that involve repetitive overhead motions can reduce strain on the shoulder.
– Stretching the shoulder and chest muscles: Regular stretching can improve flexibility and reduce tension in the shoulder and surrounding muscles, promoting better movement patterns.
– Using proper technique: Whether in sports or daily activities, ensuring proper form during overhead movements can prevent unnecessary stress on the shoulder.

Plantar Fascitis
Plantar Fascitis is a common condition where the plantar fascia, a thick band of tissue that runs along the bottom of the foot, becomes inflamed. This inflammation leads to pain, particularly in the heel, and can make walking or standing difficult. The pain is often worst in the morning or after periods of inactivity. Without treatment, plantar fasciitis can persist for months or even years, severely impacting daily activities. Below is a detailed explanation of its key aspects:
Causes
Several factors can contribute to the development of plantar fasciitis, including:
– Overuse or excessive activity: Repetitive stress from activities like running, dancing, or long periods of standing can strain the plantar fascia.
– Foot mechanics: High arches, flat feet, or an abnormal walking pattern can add strain to the plantar fascia.
– Improper footwear: Wearing shoes that lack support, especially with thin soles or poor arch support, can contribute to the condition.
– Obesity: Carrying extra weight puts additional pressure on the plantar fascia, leading to inflammation.
– Tight calf muscles or Achilles tendon: Reduced flexibility in these areas can pull on the plantar fascia, increasing the risk of injury.
Symptoms
Plantar fasciitis typically presents with the following symptoms:
1. Heel pain: Sharp, stabbing pain in the heel, particularly with the first steps in the morning or after periods of rest.
2. Pain after activity: Discomfort often increases after long periods of standing, walking, or exercise, though pain may decrease during the activity itself.
3. Stiffness and tenderness: The foot may feel tight or tender to the touch, especially along the arch and heel.
Special Tests RMTs Can Use
To assess plantar fasciitis, a Registered Massage Therapist (RMT) may perform the following tests:
– Windlass Test: This evaluates the tension in the plantar fascia by extending the big toe and observing any pain or tightness in the arch.
– Palpation: Pressing along the plantar fascia to identify areas of tenderness and inflammation.
– Gait Analysis: Observing the client’s walking pattern to identify abnormal foot mechanics that may be contributing to the condition.
– Ankle Dorsiflexion Test: Assesses flexibility in the calf muscles and Achilles tendon, which can impact plantar fascia tension.
What RMTs Can Do
RMTs can apply several techniques to alleviate pain, reduce inflammation, and promote healing in plantar fasciitis:
– Deep Tissue Massage: Targets the plantar fascia and surrounding muscles to release tension and improve circulation.
– Myofascial Release: Works on the fascia to break down adhesions and improve mobility.
– Trigger Point Therapy: Releases tight points in the calf muscles, which can contribute to plantar fascia tension.
– Cross-Friction Massage: Helps to break up scar tissue and promote healing along the plantar fascia.
– Stretching Techniques: Focuses on lengthening the calf muscles and Achilles tendon to reduce stress on the plantar fascia.
– Foot and Ankle Mobilization: Improves the range of motion in the foot and ankle joints, reducing pressure on the fascia.
Prevention
Preventing plantar fasciitis involves addressing the underlying causes and maintaining flexibility and strength in the foot and leg muscles. Key prevention strategies include:
– Wearing supportive footwear: Shoes with good arch support and cushioned soles can help reduce strain on the plantar fascia.
– Stretching: Regular stretching of the calf muscles and Achilles tendon can reduce tension on the plantar fascia.
– Strengthening exercises: Strengthening the foot and ankle muscles can improve foot mechanics and reduce stress on the plantar fascia.
– Maintaining a healthy weight: Reducing excess weight can decrease pressure on the feet.
– Avoiding overuse: Gradually increasing the intensity of physical activity and taking breaks when needed can prevent overuse injuries like plantar fasciitis.

Low Back Pain
Low back pain is a prevalent condition that affects people of all ages and lifestyles. It can result from poor posture, muscle strain, or injury and may manifest as sharp, aching, or radiating pain. Depending on the cause, it can be acute or chronic, sometimes affecting daily activities and overall mobility. Below is a detailed explanation of its key aspects:
Causes
Common causes of low back pain include:
– Muscle strain or sprain: Overstretching or tearing of muscles and ligaments due to heavy lifting, sudden movements, or poor form during exercise can lead to low back pain.
– Poor posture: Sitting or standing for long periods with improper alignment can put stress on the lower back, leading to pain and discomfort.
– Degenerative conditions: Osteoarthritis, degenerative disc disease, or herniated discs can result in chronic low back pain due to wear and tear on the spinal joints and discs.
– Injury or trauma: Falls, accidents, or sports injuries can damage the spine, muscles, or ligaments in the lower back.
– Sciatica: Compression of the sciatic nerve, often from a herniated disc, can cause pain to radiate from the lower back down the leg.
Symptoms
Low back pain can present in a variety of ways, depending on its cause:
1. Localized pain: Pain confined to the lower back, which may be sharp or aching.
2. Radiating pain: Pain that travels down one or both legs (sciatica), sometimes accompanied by numbness or tingling.
3. Stiffness: Reduced mobility and difficulty bending or twisting.
4. Muscle spasms: Sudden and painful muscle contractions that limit movement.
5. Weakness or numbness: If nerves are involved, you may experience weakness or numbness in the legs.
Special Tests RMTs Can Use
RMTs may use the following tests to assess low back pain:
– Range of Motion (ROM) Tests: Evaluates the mobility of the spine and identifies areas of tightness or discomfort.
– Straight Leg Raise Test: Assesses for sciatica or nerve root compression by raising a straightened leg while the patient is lying down.
– Palpation: Gentle pressure applied to specific areas to identify muscle spasms, tenderness, or tightness.
– Patrick’s (FABER) Test: Checks for hip joint involvement, which can sometimes contribute to lower back pain.
– Slump Test: Evaluates nerve tension and involvement, often used to diagnose sciatica.
What RMTs Can Do
RMTs can apply several techniques to relieve low back pain and restore function:
– Deep Tissue Massage: Focuses on the deeper layers of muscle tissue to release chronic tension and alleviate pain.
– Trigger Point Therapy: Targets specific points in tight muscles to relieve referred pain and improve flexibility.
– Myofascial Release: Stretches the connective tissue to improve mobility and reduce pain.
– Swedish Massage: A gentle technique that enhances circulation, reduces muscle tension, and promotes relaxation.
– Joint Mobilization: Restores movement in stiff or restricted joints, improving overall range of motion.
– Stretching and Strengthening Exercises: RMTs may recommend exercises to improve core stability, which helps support the lower back and prevent further pain.
Prevention
Preventing low back pain involves maintaining a healthy lifestyle and being mindful of body mechanics:
– Good posture: Maintain proper alignment when sitting, standing, and lifting to reduce stress on the lower back.
– Regular exercise: Strengthen the core muscles that support the spine through exercises like planks and bridges.
– Proper lifting technique: Always lift with your legs and avoid twisting your spine when carrying heavy objects.
– Stretching: Regularly stretch the hamstrings, hips, and lower back to maintain flexibility and reduce stiffness.
– Ergonomic adjustments: Ensure your workspace and sleeping environment support good posture and spinal alignment.
With proper care, prevention strategies, and treatment, low back pain can be effectively managed to improve quality of life and prevent recurrence.

General Stress
General stress is a natural response to the pressures and demands of daily life. It is not necessarily harmful in small amounts, as it can motivate action and focus. However, chronic stress can lead to physical, mental, and emotional issues, disrupting a person’s overall well-being. Below is a detailed explanation of its key aspects:
Causes
General stress can arise from a variety of sources, including:
– Work pressure: High demands, tight deadlines, or conflicts in the workplace can create ongoing stress.
– Life changes: Major transitions, such as moving, starting a new job, or relationship changes, can trigger stress.
– Financial concerns: Struggles with managing finances, debt, or job insecurity often lead to stress.
– Health issues: Personal health challenges or caring for a sick loved one can cause significant emotional and mental strain.
– Overcommitment: Juggling too many responsibilities without time for rest can overwhelm an individual.
Symptoms
The symptoms of general stress vary but commonly include:
– Physical: Headaches, muscle tension, fatigue, chest pain, or digestive problems.
– Mental: Difficulty concentrating, racing thoughts, or feeling overwhelmed.
– Emotional: Anxiety, irritability, mood swings, or feeling constantly on edge.
– Behavioral: Sleep disturbances, overeating or undereating, social withdrawal, or turning to substances like alcohol or caffeine to cope.
Special Tests RMTs Can Use
While stress itself is not diagnosed through specific tests, RMTs can assess stress-related tension and discomfort by observing:
– Postural assessments: Identifying tension in the shoulders, neck, and upper back areas, often associated with stress.
– Muscle palpation: Feeling for tight, overactive muscles, particularly in the jaw, back, and shoulders, where stress often accumulates.
– Range of motion tests: Limited movement, particularly in the neck or back, may indicate muscle tightness due to stress.
What RMTs Can Do
RMTs play an important role in alleviating stress by using various massage techniques, including:
– Swedish massage: Promotes relaxation and increases circulation, helping to reduce stress and tension in the body.
– Trigger point therapy: Focuses on relieving tight areas in the muscles that are often a result of chronic stress.
– Myofascial release: Gently stretches the fascia (the connective tissue surrounding muscles) to reduce stiffness and improve mobility.
– Aromatherapy massage: Using essential oils like lavender or eucalyptus to enhance relaxation during treatment.
– Deep tissue massage: Addresses deeper layers of muscle tension that build up from prolonged stress.
Prevention
Preventing and managing stress involves taking proactive steps to maintain balance and well-being:
– Time management: Plan and prioritize tasks to avoid feeling overwhelmed by responsibilities.
– Regular exercise: Physical activity helps relieve built-up stress and promotes a sense of calm.
– Relaxation techniques: Practices such as deep breathing, meditation, or yoga can reduce stress and promote relaxation.
– Healthy diet: Eating well-balanced meals can help stabilize energy levels and improve mood.
– Social support: Spending time with friends or family can alleviate feelings of isolation and stress.
– Sleep hygiene: Maintaining a regular sleep schedule and creating a calming bedtime routine can reduce stress and improve overall health.
With proper management techniques and support, general stress can be significantly reduced, allowing individuals to maintain better mental and physical health.

Frozen shoulder
Frozen shoulder, or adhesive capsulitis, is a condition where the shoulder becomes painfully stiff and immobile. It usually begins with increasing pain that gradually restricts shoulder movement. Over time, the joint may “freeze” entirely, making daily activities difficult. Without treatment, the condition can persist for years, and full recovery may be delayed or incomplete. Below is a detailed explanation of its key aspects:
Causes
The exact cause of frozen shoulder is not fully understood, but several factors are commonly associated with its development:
– Injury or surgery: Shoulder injuries or surgeries often lead to reduced mobility, which can cause the shoulder to stiffen.
– Medical conditions: Diabetes, thyroid disorders, cardiovascular disease, and Parkinson’s disease are known to increase the risk of developing frozen shoulder.
– Immobility: Prolonged immobility due to injury, illness, or surgery can trigger the condition.
– FOOSH (Fall On Outstretched Hand): After a fall, the rotator muscles may go into a protective spasm, leading to prolonged contraction and severe restrictions in shoulder movement. If this persists, it can result in capsular changes and progress into a frozen shoulder.
Symptoms
Frozen shoulder develops in three stages:
1. Freezing stage: Pain increases gradually, and shoulder movement becomes limited. This stage typically lasts between 6 weeks and 9 months.
2. Frozen stage: Pain may lessen, but stiffness and restricted movement become more pronounced, making everyday tasks difficult. This stage can last from 4 to 12 months.
3. Thawing stage: Shoulder movement gradually improves over 6 months to 2 years. However, full recovery may not occur without proper treatment, and long-term mobility limitations can persist.
Special Tests RMTs Can Use
To assess frozen shoulder, a Registered Massage Therapist (RMT) may conduct the following tests:
– AROM (Active Range of Motion): Evaluates joint mobility and the rotator cuff’s contractile function quality.
– PROM (Passive Range of Motion): Assesses ligament and capsular integrity of the shoulder joint.
– Empty Can Test: Checks for supraspinatus muscle involvement in the pain.
– Hawkins Test: Helps rule in or out impingement of the supraspinatus tendon.
– Painful Arc Test: Identifies weaknesses between the deltoid and supraspinatus muscles, as well as potential impingement.
– Scapular Rhythm Test: Evaluates upper trapezius compensation during shoulder abduction.
What RMTs Can Do
RMTs can apply a range of techniques to alleviate pain and restore mobility, including:
– Friction: Breaks up muscle fibers to improve circulation and increase range of motion.
– Joint Mobilization: Promotes restored mobility in joints with reduced or lost range of motion.
– Capsular Stretching: Reduces capsular adhesions that restrict shoulder movement.
– Pin & Stretch: Lengthens the internal and external rotator muscles to enhance shoulder rotation.
– Trigger Point Release: Relieves muscle tension by targeting tender points.
– Swedish Massage: Improves overall circulation, which can help alleviate pain, especially at night.
Prevention
It’s essential to maintain shoulder mobility through regular exercises to prevent frozen shoulder, especially following an injury or surgery. Managing underlying medical conditions and seeking early treatment for shoulder pain can also help reduce the risk of developing the condition.

De Quervain’s Syndrome (De Quervain’s Tenosynovitis)
De Quervain’s Syndrome, also known as De Quervain’s Tenosynovitis, is a condition where the tendons on the thumb side of the wrist become inflamed, causing pain and discomfort. It commonly affects people who perform repetitive hand and wrist motions, such as lifting, gripping, or twisting. Below is a detailed explanation of its key aspects:
Causes
De Quervain’s Syndrome is caused by irritation and inflammation of the tendons (the abductor pollicis longus and the extensor pollicis brevis) that pass through a narrow tunnel near the wrist. Common causes include:
– Repetitive wrist and thumb movements: Activities such as texting, typing, knitting, and playing musical instruments can strain the tendons.
– Overuse: Frequent lifting, especially with the thumb and wrist in awkward positions, can lead to tendon inflammation.
– Injury: Trauma or direct injury to the wrist or tendons can trigger inflammation.
– Pregnancy and hormonal changes: Fluid retention and hormonal changes during pregnancy can increase susceptibility to De Quervain’s Syndrome.
Symptoms
The primary symptom of De Quervain’s Syndrome is pain at the base of the thumb and along the wrist, which may also include:
– Pain: Pain that worsens with thumb or wrist movement, especially gripping or twisting actions.
– Swelling: Swelling at the base of the thumb, which may create a visible lump.
– Reduced Thumb Motion: Difficulty moving the thumb or wrist, especially when grasping or pinching.
– Tenderness: Sensitivity to touch along the thumb-side of the wrist.
– Crepitus: A creaking or squeaking sensation when moving the tendons.
Special Tests RMTs Can Use
RMTs can use the following tests to assess De Quervain’s Syndrome:
– Finkelstein’s Test: The patient makes a fist with the thumb inside the fingers and then bends the wrist toward the little finger. If this causes pain along the thumb side of the wrist, it indicates a positive result for De Quervain’s Syndrome.
– Eichhoff’s Test: Similar to Finkelstein’s Test but performed passively by the RMT, checking for pain in the tendons.
– Tenderness Palpation: RMT palpates the tendons at the base of the thumb to check for tenderness and swelling.
What RMTs Can Do
RMTs can apply various techniques to alleviate symptoms and promote healing in De Quervain’s Syndrome, including:
– Friction Massage: Helps break down adhesions and scar tissue in the tendons, improving circulation and reducing inflammation.
– Trigger Point Therapy: Releases tight spots in the muscles of the forearm and hand to reduce pain and tension.
– Myofascial Release: Targets the fascia around the tendons to improve flexibility and decrease restriction.
– Thumb and Wrist Stretching: Gentle stretches to improve range of motion in the thumb and wrist.
– Strengthening Exercises: Exercises to strengthen the thumb and forearm muscles, promoting better tendon stability.
– Swedish Massage: Increases overall circulation, aiding in pain relief and reducing inflammation.
– Joint Mobilization: Improves the range of motion in the wrist and thumb joints, enhancing overall function.
Prevention
Preventing De Quervain’s Syndrome involves reducing strain on the wrist and thumb tendons:
– Ergonomics: Adjust your workstation or tools to reduce repetitive strain on the wrist.
– Proper Technique: Use proper hand and wrist positioning during activities such as lifting, gripping, and typing.
– Strengthening: Strengthen the muscles in the hand, wrist, and forearm to provide better support for the tendons.
– Stretching: Regularly stretch the wrist and thumb muscles to maintain flexibility and reduce tightness.
– Rest: Take breaks during repetitive activities to give your tendons time to recover and prevent overuse injuries.
With proper care and attention to prevention, De Quervain’s Syndrome can be effectively managed, reducing pain and promoting long-term tendon health.

Carpal Tunnel Syndrome
Carpal Tunnel Syndrome (CTS) is a common condition that causes pain, numbness, and tingling in the hand and arm. It occurs when the median nerve, which runs from the forearm into the palm of the hand, becomes compressed at the wrist. The carpal tunnel is a narrow passageway on the palm side of the wrist, and when it becomes too narrow, it can cause a range of uncomfortable symptoms. Below is a detailed explanation of its key aspects:
Causes
Carpal Tunnel Syndrome is often caused by a combination of factors that put pressure on the median nerve:
– Repetitive hand use: Activities that involve repetitive hand or wrist movements, such as typing or using tools, can irritate the tendons in the wrist and cause swelling, leading to pressure on the median nerve.
– Wrist anatomy: Some people naturally have a smaller carpal tunnel, which can make them more susceptible to CTS. Fractures or dislocations in the wrist can also alter the space within the tunnel.
– Medical conditions: Conditions like diabetes, rheumatoid arthritis, and thyroid dysfunction can increase the risk of carpal tunnel by causing inflammation or swelling.
– Fluid retention: Pregnancy, menopause, or other conditions that cause fluid retention can lead to swelling in the wrist, increasing pressure on the median nerve.
– Workplace factors: Jobs that require prolonged or forceful wrist flexion, like assembly line work or heavy lifting, are associated with a higher risk of developing CTS.
Symptoms
Carpal Tunnel Syndrome typically progresses in stages:
1. Early stage: Patients may feel tingling, numbness, or burning sensations in the thumb, index, and middle fingers. Symptoms often occur at night.
2. Intermediate stage: As the condition worsens, these sensations become more frequent and may occur during the day, particularly when holding objects or performing certain activities.
3. Advanced stage: Weakness in the hand may develop, making it difficult to grasp objects or perform fine motor tasks. Without treatment, muscle deterioration around the base of the thumb can occur.
Special Tests RMTs Can Use
To assess Carpal Tunnel Syndrome, a Registered Massage Therapist (RMT) may conduct the following tests:
– Phalen’s Test: The patient holds the backs of their hands together with the wrists flexed for 60 seconds. Tingling or numbness indicates median nerve compression.
– Tinel’s Sign: The therapist taps over the carpal tunnel at the wrist. A positive test will produce tingling in the fingers.
– Two-Point Discrimination: This test evaluates the ability to differentiate between two points touching the skin. Loss of sensation may indicate nerve damage.
– Durkan’s Test (Carpal Compression Test): The therapist applies pressure directly over the carpal tunnel to see if symptoms of pain, numbness, or tingling are reproduced.
What RMTs Can Do
RMTs can help alleviate symptoms of Carpal Tunnel Syndrome through the following treatments:
– Friction massage: Breaks up adhesions in the tendons and promotes circulation to reduce inflammation.
– Myofascial release: Helps reduce tension in the fascia around the forearm and wrist, relieving pressure on the median nerve.
– Stretching: Targeted stretches for the forearm flexor and extensor muscles help to restore flexibility and reduce compression on the carpal tunnel.
– Trigger Point Therapy: Relieves tension in associated muscles like the flexor carpi radialis and flexor digitorum by targeting specific points of discomfort.
– Nerve gliding exercises: These exercises promote healthy movement of the median nerve through the carpal tunnel, reducing the risk of it becoming trapped.
– Joint Mobilization: Gentle mobilization of the wrist joint can increase the range of motion and improve the overall function of the hand and wrist.
Prevention
Preventing Carpal Tunnel Syndrome involves reducing strain on the wrist and maintaining good hand ergonomics:
– Modify repetitive activities: Take breaks during activities that require repetitive wrist motions, such as typing or using tools.
– Ergonomic adjustments: Ensure proper wrist positioning during activities. For instance, keep wrists in a neutral position when typing and use ergonomic tools to minimize strain.
– Exercises and stretches: Regularly perform hand and wrist stretches to maintain flexibility and reduce the risk of median nerve compression.
– Manage underlying health conditions: Properly managing conditions like diabetes, arthritis, or thyroid issues can lower the risk of developing CTS.

Achilles Tendonitis
Achilles tendonitis is a condition where the Achilles tendon, which connects the calf muscles to the heel bone, becomes inflamed. It is commonly caused by overuse or repetitive strain, especially in activities that involve running, jumping, or sudden changes in speed. Below is a detailed explanation of its key aspects:
Causes
Achilles tendonitis is typically caused by repetitive stress on the tendon, leading to inflammation and degeneration. Common causes include:
– Overuse: Running, jumping, or high-impact activities can strain the Achilles tendon, especially if performed without adequate warm-up or conditioning.
– Improper footwear: Shoes that lack proper support or cushioning can place excessive stress on the Achilles tendon.
– Sudden increase in activity: Rapidly increasing the intensity or duration of physical activity without gradually conditioning the body can lead to tendonitis.
– Tight calf muscles: Tight or inflexible calf muscles can increase tension on the Achilles tendon, leading to inflammation.
– Flat feet or high arches: Structural foot problems can affect how stress is distributed across the tendon during movement, increasing the risk of injury.
Symptoms
The primary symptoms of Achilles tendonitis include:
– Pain: Aching or sharp pain along the back of the heel, especially during or after physical activity. The pain is often worse in the morning or after periods of rest.
– Tenderness: Sensitivity to touch along the Achilles tendon, particularly when pressing on the area.
– Stiffness: Difficulty flexing the foot or ankle, especially after waking up or resting for extended periods.
– Swelling: Visible swelling or thickening of the tendon due to inflammation.
– Limited mobility: Reduced ability to push off the foot or fully extend the ankle during activities like walking or running.
Special Tests RMTs Can Use
RMTs can use the following tests to assess Achilles tendonitis:
– Thompson Test: The patient lies face down while the RMT squeezes the calf muscle. A lack of movement in the foot suggests an Achilles tendon injury.
– Palpation: The RMT palpates along the length of the Achilles tendon to identify areas of tenderness, swelling, or thickening.
– Dorsiflexion Test: The patient flexes the foot upward, and the RMT assesses the range of motion and whether pain occurs during the stretch.
What RMTs Can Do
RMTs can apply various techniques to alleviate Achilles tendonitis symptoms and promote healing, including:
– Friction Massage: Breaks down scar tissue and adhesions in the tendon to promote circulation and healing.
– Trigger Point Therapy: Targets tight spots in the calf muscles to reduce tension on the Achilles tendon.
– Myofascial Release: Loosens the fascia surrounding the calf muscles, promoting flexibility and reducing strain on the tendon.
– Stretching and Strengthening Exercises: Gentle stretching and strengthening exercises help improve the flexibility and resilience of the calf muscles and Achilles tendon.
– Swedish Massage: Promotes relaxation and improves circulation, aiding in the reduction of inflammation and pain.
– Joint Mobilization: Enhances ankle joint function and range of motion by mobilizing surrounding structures.
Prevention
Preventing Achilles tendonitis involves taking steps to reduce stress on the tendon:
– Proper footwear: Wear shoes that provide good support and cushioning, especially during physical activity.
– Stretching: Regularly stretch the calf muscles to maintain flexibility and reduce tension on the Achilles tendon.
– Gradual progression: Increase the intensity and duration of physical activities gradually to avoid overloading the tendon.
– Strengthening exercises: Strengthen the calf muscles and lower leg to support the Achilles tendon and improve its resilience.
– Warm-up and cool-down: Always warm up before physical activity and cool down afterward to reduce the risk of injury.
– Rest: Take breaks from repetitive or high-impact activities to allow the tendon time to recover.
With proper care and preventative measures, Achilles tendonitis can be effectively managed, reducing pain and preventing further injury.

Golfer’s Elbow (Medial Epicondylitis)
Golfer’s elbow, or medial epicondylitis, is a condition where the tendons on the inner side of the elbow become inflamed, leading to pain and weakness. While it’s commonly associated with golfers, it can affect anyone who repeatedly overuses their forearm muscles. Below is a detailed explanation of its key aspects:
Causes
Golfer’s elbow is caused by repetitive stress and overuse of the forearm muscles, leading to small tears in the tendons that attach to the medial epicondyle (the inner part of the elbow). Common causes include:
– Repetitive arm movements: Activities such as golf, throwing, gripping, and using hand tools can strain the forearm muscles and tendons.
– Improper technique: Poor form in activities like golfing, racket sports, or weightlifting can place additional stress on the elbow tendons.
– Age: Golfer’s elbow is more common in people aged 40 and older, as tendons lose flexibility and are more prone to injury with age.
Symptoms
The primary symptom of golfer’s elbow is pain on the inside of the elbow, but it may also include:
– Pain or tenderness: Discomfort radiating from the inner elbow down the forearm, particularly during gripping, lifting, or wrist flexing.
– Weakness: Reduced strength in the forearm, making it harder to grip objects or hold items.
– Stiffness: Difficulty fully bending or straightening the elbow, especially in the morning or after rest.
– Numbness or tingling: Sensations may radiate to the fingers, particularly the ring and little fingers.
Special Tests RMTs Can Use
RMTs may use the following tests to assess golfer’s elbow:
– Resisted Wrist Flexion Test: The patient resists wrist flexion while the RMT palpates the medial epicondyle to check for pain.
– Palpation of the Medial Epicondyle: The RMT presses on the inner elbow to detect tenderness in the tendons.
– Golfer’s Elbow Test: The patient extends their elbow while the RMT flexes the wrist and fingers to assess for pain along the inner elbow.
What RMTs Can Do
RMTs can apply various techniques to alleviate golfer’s elbow symptoms and promote healing, including:
– Friction Massage: Breaks down adhesions and scar tissue in the tendons to improve circulation and healing.
– Trigger Point Therapy: Targets tight spots in the forearm muscles to release tension and reduce pain.
– Myofascial Release: Relieves tension in the fascia surrounding the muscles and tendons, improving flexibility and mobility.
– Stretching and Strengthening Exercises: Gentle exercises that enhance tendon flexibility and strengthen the muscles to reduce strain.
– Swedish Massage: Improves overall blood circulation, which helps decrease inflammation and pain.
– Joint Mobilization: Restores range of motion and improves the function of the elbow joint by mobilizing surrounding structures.
Prevention
Preventing golfer’s elbow involves minimizing strain on the forearm muscles and tendons by:
– Proper technique: Ensure correct form in sports or work-related tasks to reduce stress on the elbow.
– Strengthening exercises: Strengthen the forearm muscles to better handle repetitive motions.
– Stretching: Regular stretching of the forearm muscles helps maintain flexibility and prevent tightness.
– Ergonomics: Adjust tools, equipment, or workstations to reduce pressure on the elbow.
– Rest: Allow the elbow and forearm muscles time to recover after repetitive or high-intensity activities to prevent overuse injuries.
With proper care and prevention, golfer’s elbow can be effectively managed, reducing pain and preventing long-term tendon damage.

Tennis Elbow
Tennis elbow, or lateral epicondylitis, is a condition where the tendons on the outside of the elbow become inflamed, leading to pain and weakness. It is not exclusive to tennis players and can affect anyone who repeatedly overuses their forearm muscles.
Causes
Tennis elbow is caused by repetitive stress and overuse of the forearm muscles, leading to tiny tears in the tendons that attach to the lateral epicondyle (the outer part of the elbow). Common causes include:
– Repetitive arm movements: Activities such as tennis, painting, typing, and using tools can strain the forearm muscles and tendons.
– Improper technique: In sports like tennis or activities that involve gripping and twisting, improper technique or equipment can increase the strain on the elbow tendons.
– Age: Tennis elbow is most common between the ages of 30 and 50, as tendons become less flexible and more prone to injury with age.
Symptoms
The primary symptom of tennis elbow is pain on the outside of the elbow, but it may also include:
1. Pain or burning: Pain radiating from the outer elbow down the forearm, especially during gripping, lifting, or twisting motions.
2. Weakness: Decreased strength in the forearm, making it difficult to hold or lift objects.
3. Tenderness: Sensitivity to touch around the outer elbow.
4. Stiffness: Difficulty fully extending the elbow in the morning or after rest.
Special Tests RMTs Can Use
RMTs may use the following tests to assess tennis elbow:
– Cozen’s Test: The patient resists wrist extension while the RMT palpates the lateral epicondyle, assessing for pain in the tendon.
– Mill’s Test: The patient extends their elbow and flexes their wrist downward while the RMT checks for pain along the outer elbow.
– Maudsley’s Test: The patient extends the middle finger against resistance, checking for pain at the lateral epicondyle.
– Grip Strength Test: Evaluates for weakness or discomfort during gripping motions.
What RMTs Can Do
RMTs can apply various techniques to alleviate tennis elbow symptoms and promote healing, including:
– Friction Massage: Breaks down scar tissue and adhesions in the tendons to improve circulation and aid in healing.
– Trigger Point Therapy: Targets tight areas in the forearm muscles to release tension and reduce pain.
– Myofascial Release: Relieves tension in the fascia surrounding the muscles and tendons, promoting mobility.
– Stretching and Strengthening Exercises: Gentle stretches and specific strengthening exercises to improve flexibility and reduce strain on the tendons.
– Swedish Massage: Promotes relaxation and overall circulation, which can assist in reducing inflammation and pain.
– Joint Mobilization: Enhances the range of motion and function of the elbow joint by mobilizing the surrounding structures.
Prevention
Preventing tennis elbow involves managing the strain on your forearm muscles and tendons:
– Proper technique: Ensure correct form when performing repetitive arm movements, whether in sports or work-related tasks.
– Strengthening exercises: Strengthen the forearm and wrist muscles to better handle repetitive motions.
– Stretching: Regularly stretch the forearm muscles to maintain flexibility and prevent tightness.
– Ergonomics: Adjust your workstation or sporting equipment to reduce strain on the elbow tendons.
– Rest: Give your elbow and forearm muscles time to recover after intense or repetitive activities to prevent overuse injuries.
With appropriate care and preventative strategies, tennis elbow can be managed effectively, reducing pain and preventing long-term damage to the tendons.